Research Article
Perception and Attitude Towards Interdisciplinary Approach to Patient Care
- Iyevhobu Kenneth Oshiokhayamhe 1,23*
1Department of Medical Microbiology, Faculty of Medical Laboratory Science, Ambrose Alli University, Ekpoma, Edo State, Nigeria.
2Department of Medical Laboratory Science, Edo State University Iyamho, Edo State, Nigeria.
3Saint Kenny Diagnostic and Research Centre, Ekpoma, Edo State, Nigeria.
*Corresponding Author: Iyevhobu Kenneth Oshiokhayamhe, Department of Medical Microbiology, Faculty of Medical Laboratory Science, Ambrose Alli University, Ekpoma, Edo State, Nigeria.
Citation: Oshiokhayamhe IK. (2026). Perception and Attitude Towards Interdisciplinary Approach to Patient Care, International Journal of Biomedical and Clinical Research, BioRes Scientia Publishers. 6(4):1-11. DOI: 10.59657/2997-6103.brs.26.123
Copyright: © 2026 Iyevhobu Kenneth Oshiokhayamhe, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: January 27, 2026 | Accepted: February 27, 2026 | Published: March 06, 2026
Abstract
Interdisciplinary approach increases productivity, contributes to the better use of team members’ skills and leads to a greater feeling of individual responsibility for achieving the objective, as well as ensures holistic patient care, stimulates creativity and results in innovative solutions in patient care. The main objective of this study is to determine the perception and attitudes of healthcare workers towards interdisciplinary approach to patients care in Asaba specialist hospital. This study adopted the cross-sectional design to determine perception and attitudes of healthcare workers towards interdisciplinary approach to patients care in Asaba specialist hospital. The population for this study consisted of 545 healthcare workers which include doctors, nurses, pharmacist, laboratory scientist, and others in Asaba specialist hospital. 65 medical doctors, 326 nurses or midwives (registered and technicians), 59 laboratory scientists, 95 others (physiotherapists, pharmacists, and radiographers). Stratified sampling technique using the class list will be used to select health care workers in Asaba specialist hospital. On the age, the respondents in their 20s had the highest number of 138(48.42%) followed by those in their 40s 60(21.05%) with the least been respondents in 50s 32(11.23%). Most of the respondents were males 153(53.68%). About 171(60%) of the health workers were nurses, 34(11.93%) were medical doctors, 30(10.53%) were medical laboratory scientists while 50(17.54%) belong to other professions. Further analysis of the professional experience, age group, experience and profession revealed the following: most of the respondents 100(35.09%) had >5 years’ experience, 75(26.32%) had 3-4 years’ experience, 60(21.05%) had 1-2 years’ experience while 50(17.54%) had <1 year experience. To illustrate this point, 22.11% of the participants agreed and 26.32% of them strongly agreed with the statement of “Interprofessional approach makes the delivery of care more efficient”. Analysis of participants’ responses to each statement shows that; most of the respondents 38.95% agree that “team approach permits health professionals to meet the needs of family caregivers as well as patients”. About 29.82% strongly agreed, 15.79% agreed, 20.35% disagreed while 14.73% strongly disagreed that “working on a team keeps most health professionals enthusiastic and interested in their jobs”. This study found that health care professionals at the specialist hospital appropriate interdisciplinary approach to patient care. To ensure the integration of care, the authors of this current study recommend that facility management hosts awareness campaigns, regarding the transition from referral to collaboration. Interdisciplinary approach is increasingly employed to treat patients.
Keywords: perception; attitude; interdisciplinary; approach; patient care
Introduction
The World Health Organization (WHO) defines a team as a group of two or more individuals who interact dynamically, independently and adaptively towards a common and valued goal or mission, and who have been assigned specific roles or functions to perform at a specified time (Gyory et al., 2019). In healthcare, teams are frequently formed to address challenging clinical issues by means of introducing innovative solutions. The underlying rationale is the fact that the decisions and actions undertaken by the team should more effectively resolve multidimensional issues.
Interdisciplinary teams are characterized by a greater overlap of professional roles, formal and informal communication and joint problem solving for the benefit of the patient. Professionals cooperating in interdisciplinary teams rely on expert opinion from each discipline, which results in the creation of common patient goals (Kelly et al., 2019). Improving the healthcare system requires simultaneous pursuit of four goals: enhancing the quality of care provided, improving the population’s health status, reducing healthcare costs and increasing job satisfaction among healthcare professionals (Bachynsky, 2020). Numerous studies indicate that the above-mentioned goals may be achieved by means of various approach of the interdisciplinary teams. As pointed out by Dumlao (2023), interdisciplinary approach increases productivity, contributes to the better use of team members’ skills and leads to a greater feeling of individual responsibility for achieving the objective, as well as ensures holistic patient care, stimulates creativity and results in innovative solutions in patient care. The WHO (2019) in their report stated that interdisciplinary approach was associated with better outcomes in the areas of family medicine, treatment and control of infectious disease, as well as humanitarian relief.
Recently, the healthcare delivered through complicated systems that involve patients interacting with healthcare professionals, each with separate and important knowledge, technical skills, and perspectives which is difficult for a single profession to be able to solve various problems and complicated issues and to accomplish the task of optimum standard patient/client care. This made the policymakers look for innovative strategies and ideas that can help them develop policies and concepts to bolster the global health workforce. One of the highlighted recommendations suggested that the healthcare professionals should progressively inspired to work as a team in delivering care for patients (Muthuri et al., 2020). When healthcare providers practically work collaboratively, they obtain common goals and are ready to analyze and fix any issues that arise. They create higher use of their skills and knowledge and they are able to coordinate care according to patients’ needs more effectively. As a result, patients ought to receive higher quality care.
Additionally, to enhancing quality care, interdisciplinary approach contributes to job satisfaction for the healthcare provider and this can be referred to interprofessional practice (IPP). Now, a good teamwork is globally recognized as a necessary tool for constructing a more effective and patient centered health care supply system (Spoorthy et al., 2020). The modern health care system has become exceedingly complex and specialized with a spread of various health care professionals working together to assist consumers address their health problems. Frequently, the most severe health threats, consisting of invasive cancers, heart disease, and HIV/AIDS call for close coordination from different health care workers (such as nurses, pharmacists, therapists, social workers, surgeons, oncologists, cardiologists, anesthesiologists, and internal medicine physicians) (Singh et al., 2019).Team members contribute specialized knowledge and skills toward addressing complex health care challenges in order that, the team members should be ready to use strategic communication to reinforce health outcomes and supply quality care to patients and their families. Health communication strategies must be developed within health care teams to market cooperation between team members, to share relevant information and to push coordination in making relevant health decisions (Mheidly & Fares, 2020).
In Nigeria, anecdotal evidence shows that clinical services are often organized along strict professional lines and teams are formed by and within individual professions independent of one another. Consultant-led obstetrics and gynecology teams (units), for instance, are made up of doctors only and deliver services along strict professional lines. Nursing care is often organized according to wards and clinics, and complements the medical care in those wards and clinics. Similarly, pharmacy and laboratory services function almost completely independently. Collaboration among these groups occurs only to the extent that each group carries out its functions to permit patient care to proceed in a coordinated fashion. A semblance of interdisciplinary teams can be found only in high dependency units such as accident and emergency departments, labor wards, intensive care units, and newborn special care units.
Several studies related to collaborative practice have been conducted in Africa (Manyama et al., 2020; Opele, 2022). Manyama et al (2020) studied pharmacists in Limpopo province in South Africa and found that 95% of respondents reported that they were not engaged in meetings or ward rounds with other healthcare workers. Similarly, Opele, (2022) conducted a study of physician or nurse collaboration in Nigeria and reported that 80% of the doctors showed poor attitudes to doctor–nurse collaboration; however, 84% of the nurses had a good attitude towards doctor–nurse collaboration.
The frameworks for clearer understanding of the practice of interdisciplinary approach in the context of interprofessional teamwork are many, but the concepts are similar and interrelated. The team-based care framework, as developed by Spaulding et al., (2021) (Sibbald et al., 2022), have been successfully applied by other researchers in studying interdisciplinary approaches in various health care settings (Sibbald et al., 2022). The framework is based on four core domains or elements that are each linked in two-way patterns to the centrally positioned interprofessional collaborative team group. These core domains are the (a) relational factors, which pertains to team relationship issues of power, hierarchy, leadership, roles and (b) processes, processual factors that focuses on the systematic processes of collaboration such as time, space, routines, rituals, information and communication technology, and task shifting; (c) organizational factors, which include institutional structures, management processes, supports or litigation postures; and the (d) contextual factors, that relate to sociocultural, socioeconomic, and political environment of the organization (Sibbald et al., 2022).
The extent of the practice of interdisciplinary approach in the Nigerian healthcare settings within the practice environment has not been fully described. Many resource-rich countries have successfully implemented interdisciplinary approach with varied levels of success in the delivery of primary healthcare (Onyedibe et al., 2020).
No studies that specifically evaluated healthcare workers’ perceptions and attitude of interdisciplinary approach were identified. It is not clear how healthcare workers perceive and respond to interdisciplinary approach in their work place. Therefore, this research was conducted to assess the perceptions and attitude of healthcare workers in this regard. A clear understanding of healthcare workers’ perceptions and attitude on interdisciplinary approach is an important step towards improvement of healthcare workers’ performance and delivery of a patient care. The results of this study will help identify strategies to promote interdisciplinary approach at the largest tertiary and academic hospital in Asaba Specialist Hospital. Despite the long history and even recent high expansion of medical education in Nigeria in the last two decades, unfortunately, no published literature concerning interdisciplinary approach in practice and in education and we have no idea about their perception and attitude toward the interdisciplinary approach in patient care. Internationally, the World Health Organization (WHO) recognized the importance of interdisciplinary approach and launched its Framework for Action on interprofessional training as a guide for implementation, in 2010 (Bogossian et al., 2023).
So there is a need to explore the different dimensions of interdisciplinary approach from health care workers and it supposed to provide a data base and records to encourage the policy makers to recognize its importance and look for innovative strategies and ideas that can help them implement the interdisciplinary approach in Asaba specialist hospital in concordance to community situation and needs and interdisciplinary approach among all professionals to improves their collaboration and help them to take necessary actions to solve problem in patient care.
Therefore, the problem was that, while the standard practice of interdisciplinary approach is known globally and has been successfully and beneficially implemented in all levels of healthcare in the resources-rich countries, the practice of interdisciplinary approach of patient care have not been clearly described in the Nigerian healthcare settings. The main objective of this study is to determine the perception and attitudes of healthcare workers towards interdisciplinary approach to patients care in Asaba specialist hospital.
Methodology
Research Design
This study adopted the cross-sectional design to determine perception and attitudes of healthcare workers towards interdisciplinary approach to patients care in Asaba specialist hospital.
Research Setting
Asaba is the capital city of Delta State, Nigeria. It is located at the western bank of the Niger River, in the Oshimili South Local Government Area. Asaba had a population of 149,603 as at the 2006 census, and a metropolitan population of over half a million people (asaba.com, 2016). The Asaba specialist hospital is a public hospital, located at Okpanam/Ugbolu, Oshimili North Local Government, Delta State. It was established on 5/2/2019, and operates on 24hrs basis. The Asaba specialist hospital is Licensed hospital by the Nigeria Ministry of Health, with facility code 10/14/1/2/1/0011 and registered as Secondary Health Care Centre.
Target Population
The population for this study consisted of 545 healthcare workers which include doctors, nurses, pharmacist, laboratory scientist, and others in Asaba specialist hospital. 65 medical doctors, 326 nurses or midwives (registered and technicians), 59 laboratory scientists, 95 others (physiotherapists, pharmacists, and radiographers).
Sample Size Determination
The sample size of the study is calculated by using the slovin’s formula.
Slovin’s formula.
(e=0.05) margin of error.
The following formula was used for calculating sample size:
The Slovin’s formula is:
n= N/ (1+N.e2)
Where: (n=sample size, N=population size, E=desired margin of error).
The sample size will be
n= N/ (1+N.e2)
n=545/ (1+545.0.05^2) =231.
10% attrition was added to give n= 285
Sample Technique
Stratified sampling technique using the class list will be used to select health care workers in Asaba specialist hospital. The health care workers who meet the inclusion criteria were encouraged to participate because they had been exposed to patient care to be able to comment on a variety of situations according to their experiences.
Inclusion Criteria
This study will include the following: Health care workers working in Asaba specialist hospital, Male and Female health care workers and health care workers able to read and write in English and willing to consent to participate in the study.
Exclusion Criteria
Health care workers working in other hospitals.
Instrument for Data Collection
In Asaba Specialist Hospital, the research tool included sociodemographic data of participating health care worker (gender, age) as well as a profile (level of education, years of experience experience) were also collected. Total of two hundred and eighty-five (285) participating health care workers completed a self-administered questionnaire - the Perception of Interprofessional Collaboration Model Questionnaire (PINCOM) - and a self-structured questionnaire. The model Contains 20 questions. The scale composed of three dimensions assessing individual, group and organizational collaborations, each measured by four constructs (subscales) ranging in 5 points from strongly agree to strongly disagree. Some questions were added to origin questionnaire in individual aspect. Also, we added about 10 questions to attitude aspect.
Validity of the Research Instrument
The researcher used a Donabedian Model structured questionnaire for data collection for this study. It was face validated by three expert opinions with no major modifications. A pilot study was carried out on 29 health care workers (10% of study population) in Asaba specialist hospital before the study to assess the feasibility and reliability of the questionnaire.
Reliability of the Research Instrument
A copy of the survey questions was sent to a senior Professor for review and revisions prior to distribution of the forms to ensure the accuracy of the data. The reliability coefficient, which was 0.79 showed the instrument's good level of dependability.
Method of Data Collection
The data needed for the study was collected through the use of researcher administered questionnaires. A cover letter to respondents was added to ensure prospective respondents were well informed on the purpose of the research exercise and also the confidentiality of the respondents in participating in the study. The questionnaire was administered and collected with the help of the three research assistants, in the space of three weeks to two weeks to health care workers in Asaba.
Method of Data Analysis
Data will be coded, collated and tabulated by the researcher. Thereafter, it was analyzed using simple descriptive data analysis of frequencies and percentages. The result was presented in tables. The data firstly summarized numerically (mean, standard deviation, median) and graphically (frequency tables and graphics) through statistical package for social sciences SPSS version 23 (SPSS, Chicago, IL, USA) to estimate and describe the perception of nurses toward Inter professional Practice. Exploratory factor analysis (Principal Component Analysis) and reliability analyses were used to explore features of the modified PINCOM-Q. Chi-square tests used to test association among variables Finally t test- sample was used to compare means and chi-square tests used to test association among variables. All the statistical test will be considered as statistically significant when p less than 0.05.
Ethical Consideration
Ethical clearance will be obtained from the Ethics and research center of Asaba specialist Hospital, Asaba prior to the start of study. Participants were informed about the objectives and stated that the participation was purely voluntary. The participant’s consent to participate in the study was implied when they tick yes to answer the questionnaire, and they had complete freedom either to decline or answer the questionnaire. To overcome Response bias and information bias in the study we used neutrally worded words, avoided the leading questions and keeping researcher’s identity anonymous. The health worker’s privacy and confidentiality were strictly maintained throughout the study.
Results
Two hundred and eighty-five health care workers were administered with questionnaires within the period and 237 (83.43%) completed the questionnaire survey. Hence, 237 health professionals were recruited into the study. Table 1 presents the demographic characteristics of the respondents. On the age, the respondents in their 20s had the highest number of 138(48.42%) followed by those in their 40s 60(21.05%) with the least been respondents in 50s 32(11.23%). Most of the respondents were males 153(53.68%). About 171(60%) of the health workers were nurses, 34(11.93%) were medical doctors, 30(10.53%) were medical laboratory scientists while 50(17.54%) belong to other professions. Further analysis of the professional experience, age group, experience and profession revealed the following: most of the respondents 100(35.09%) had >5 years’ experience, 75(26.32%) had 3-4 years’ experience, 60(21.05%) had 1-2 years’ experience while 50(17.54%) had less than 1 year experience.
Table 1: Socio demographics of respondents.
| Characteristics | Frequency (n=285) | Percentage (%) |
| Age group (years) | ||
| 20s | 138 | 48.42 |
| 30s | 55 | 19.30 |
| 40s | 60 | 21.05 |
| 50s | 32 | 11.23 |
| Total | 285 | 100 |
| Sex | ||
| Male | 153 | 53.68 |
| Female | 132 | 46.32 |
| Total | 285 | 100 |
| Health Workers | ||
| Nurses | 171 | 60 |
| Doctors | 34 | 11.93 |
| Laboratory Scientist | 30 | 10.53 |
| Others | 50 | 17.54 |
| Total | 285 | 100 |
| Level of Education | ||
| Diploma | 95 | 33.33 |
| Bachelor’s degree | 85 | 29.82 |
| Master’s degree | 68 | 23.68 |
| Doctorate’s degree | 37 | 12.98 |
| Years of Experience | ||
| Total | 285 | 100 |
| less than 1year | 50 | 17.54 |
| 1-2years | 60 | 21.05 |
| 3-4years | 75 | 26.32 |
| >5years | 100 | 35.09 |
| Total | 285 | 100 |
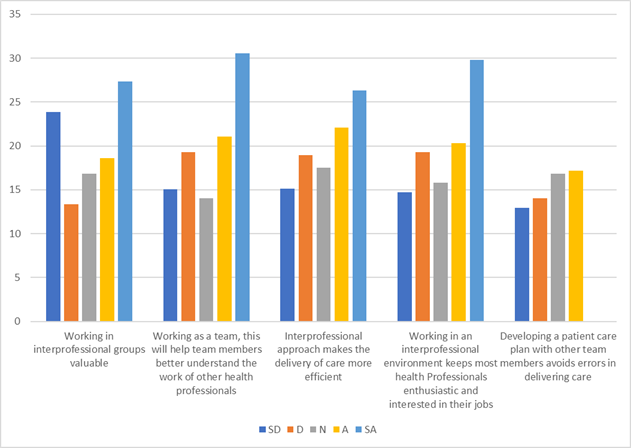
This three-subscale consisted of five statements to measure participants’ perception of interprofessional approach. To illustrate this point, 22.11% of the participants agreed and 26.32% of them strongly agreed with the statement of “Interprofessional approach makes the delivery of care more efficient”. Additionally, the statement “Working in interprofessional groups valuable” had 20.35% agreement and 29.82% strong agreement. The percentage of participants who agreed (15.79%) and disagreed (19.65%) with the statement based on the group subscale was almost the same “professionals are good at exchanging information with each other about how they work”. The percentage of participants who strongly agreed (15.79%), agreed (19.65%), strongly disagreed (24.91%) and disagreed (20.35%) with the statement based on the group subscale was almost the same “there’s always good communication in interprofessional groups”. However, a large proportion of the respondents strongly disagree (26.32%) while 21.03% disagreed with the statement “interprofessional practicing is important but cannot be applied in Asaba Specialist Hospital.”
Table 2: Perception of health workers towards interdisciplinary approach to patient care.
| Variables | SD | D | N | A | SA |
| Individual Aspect | |||||
| Working in interprofessional groups valuable | 23.86 | 13.33 | 16.84 | 18.60 | 27.37 |
| Working as a team, this will help team members better understand the work of other health professionals | 15.09 | 19.30 | 14.03 | 21.05 | 30.53 |
| Interprofessional approach makes the delivery of care more efficient | 15.10 | 18.95 | 17.54 | 22.11 | 26.32 |
| Working in an interprofessional environment keeps most health Professionals enthusiastic and interested in their jobs | 14.73 | 19.30 | 15.79 | 20.35 | 29.82 |
| Developing a patient care plan with other team members avoids errors in delivering care | 12.95 | 14.04 | 16.84 | 17.19 | 38.95 |
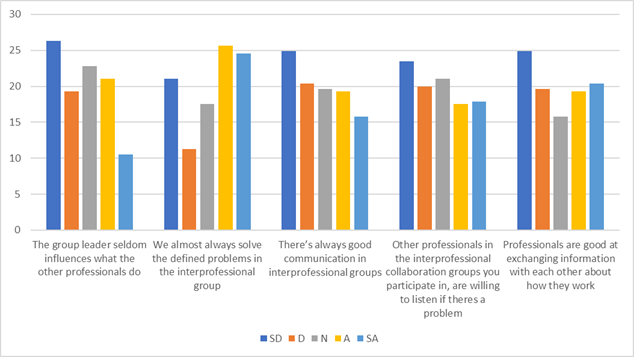
| Group Aspect | |||||
| The group leader seldom influences what the other professionals do | 26.32 | 19.30 | 22.81 | 21.05 | 10.53 |
| We almost always solve the defined problems in the interprofessional group | 21.05 | 11.23 | 17.54 | 25.61 | 24.56 |
| There’s always good communication in interprofessional groups | 24.91 | 20.35 | 19.65 | 19.30 | 15.79 |
| Other professionals in the interprofessional collaboration groups you participate in, are willing to listen if there is a problem | 23.51 | 20.00 | 21.05 | 17.54 | 17.90 |
| Professionals are good at exchanging information with each other about how they work | 24.91 | 19.65 | 15.79 | 19.30 | 20.35 |
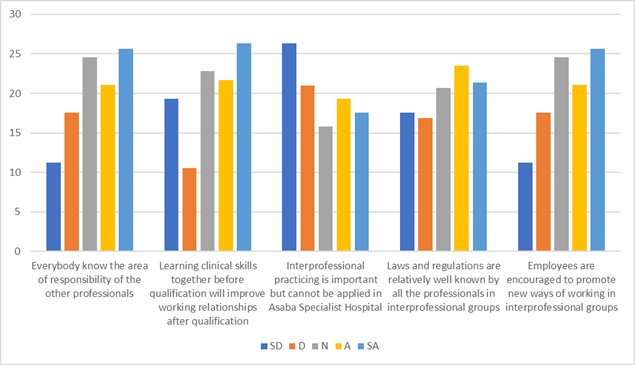
| Organizational Aspect | |||||
| Everybody knows the area of responsibility of the other professionals | 11.23 | 17.54 | 24.56 | 21.05 | 25.61 |
| Learning clinical skills together before qualification will improve working relationships after qualification | 19.30 | 10.53 | 22.81 | 21.65 | 26.32 |
| Interprofessional practicing is important but cannot be applied in Asaba Specialist Hospital. | 26.32 | 21.03 | 15.79 | 19.30 | 17.54 |
| Laws and regulations are relatively well known by all the professionals in interprofessional groups | 17.54 | 16.84 | 20.70 | 23.51 | 21.40 |
| Employees are encouraged to promote new ways of working in interprofessional groups | 11.23 | 17.54 | 24.56 | 21.05 | 25.61 |
Table 3 summarises the health care workers responses to the 14 items on the table chart. Analysis of participants’ responses to each statement shows that; most of the respondents 38.95% agree that “team approach permits health professionals to meet the needs of family caregivers as well as patients”. About 29.82% strongly agreed, 15.79% agreed, 20.35% disagreed while 14.73% strongly disagreed that “working on a team keeps most health professionals enthusiastic and interested in their jobs”. Most of the study respondents strongly agreed (30.53%) that “having to report observations to the team helps team members better understand the work of other health professionals”. Most of the study respondents 26.32% disagreed that “team approach makes the delivery of care more efficient”. 38.95%, 29.82% and 27.37% of the study respondents strongly agreed that “team approach improves the quality of care to patients”, “patients receiving team care are more likely than other patients to be treated as whole persons” and “The give and take among team members helps them make better patient care decisions” respectively. Most of the study respondents 27.37% and 38.95% strongly disagreed that “Hospital patients who receive team care are better prepared for discharge than other patients” and “In most instances, the time required for team meetings could be better spent in other ways” respectively. Most of the study respondents 29.82%, 26.32% and 38.95% of the study respondents strongly agreed that “Developing a patient care plan with other team members avoids errors in delivering care”, “Team meetings foster communication among team members from different disciplines” and “Health professionals working on teams are more responsive than others to the emotional and financial needs of patients” respectively. While most of the study respondents 30.53% and 27.37% of the study respondents strongly disagreed that “Working in teams unnecessarily complicates things most of the time” and “Developing an interdisciplinary patient care plan is excessively time-consuming” respectively.
Table 3: Attitudes of health care workers towards interdisciplinary approach to patient care.
| Statement | SD | D | N | A | SA |
| The team approach permits health professionals to meet the needs of family caregivers as well as patients | 14.04 | 17.19 | 16.84 | 38.95 | 12.98 |
| Working on a team keeps most health professionals enthusiastic and interested in their jobs | 14.73 | 20.35 | 19.30 | 15.79 | 29.82 |
| Having to report observations to the team helps team members better understand the work of other health professionals | 15.09 | 21.05 | 19.30 | 14.03 | 30.53 |
| The team approach makes the delivery of care more efficient | 22.81 | 26.32 | 21.05 | 15.79 | 19.30 |
| The team approach improves the quality of care to patients | 14.04 | 17.19 | 16.84 | 12.98 | 38.95 |
| Patients receiving team care are more likely than other patients to be treated as whole persons | 14.73 | 20.35 | 19.30 | 15.79 | 29.82 |
| The give and take among team members help them make better patient care decisions | 23.86 | 13.33 | 16.84 | 18.60 | 27.37 |
| Hospital patients who receive team care are better prepared for discharge than other patients | 27.37 | 23.86 | 13.33 | 16.84 | 18.60 |
| In most instances, the time required for team meetings could be better spent in other ways | 38.95 | 17.19 | 14.04 | 16.84 | 12.98 |
| Developing a patient care plan with other team members avoids errors in delivering care | 14.73 | 15.79 | 19.30 | 20.35 | 29.82 |
| Team meetings foster communication among team members from different disciplines | 19.30 | 15.79 | 21.05 | 22.81 | 26.32 |
| Health professionals working on teams are more responsive than others to the emotional and financial needs of patients | 14.04 | 17.19 | 16.84 | 12.98 | 38.95 |
| Working in teams unnecessarily complicates things most of the time | 30.53 | 21.05 | 14.03 | 15.09 | 19.30 |
| Developing an interdisciplinary patient care plan is excessively time-consuming | 27.37 | 23.86 | 13.33 | 18.60 | 16.84 |
Figure 1: Individual Aspect: Perception of health workers towards interdisciplinary approach to patient care.
Figure 2: Group Aspect: Perception of health workers towards interdisciplinary approach to patient care.
Figure 3: Organizational Aspect: Perception of health workers towards interdisciplinary approach to patient care.
The perception of health care workers towards interdisciplinary approach to patient care was found to be positive. This goes on to say that working as a team is highly appreciated. The attitudes of healthcare workers towards interdisciplinary approach to patients care in Asaba specialist hospital was found to be highly positive.
Discussion
This study assessed the perception and attitudes of health care workers towards interdisciplinary approach to patient in Asaba Specialist teaching hospitals. Generally, most participants agreed (or strongly agreed) with the positively worded statements with relatively fewer agreeing with the three negatively worded statements on the 14-item scale. The perception and attitude of health care professionals towards interdisciplinary approach to patient differed significantly by age, profession, facility, and professional experience.
Analysis of the health care workers responses to the 14 items on the scale revealed that the majority (64.29%) of the practitioners felt that interdisciplinary approach would be beneficial to the patient. Most (38.95%) professionals disagreed with the negatively worded statements on the time requirements for interdisciplinary collaboration, except for the statement on developing an interdisciplinary patient care plan where over 40% were neutral in their responses, indicating they were not certain of the time demands of this care plan prior to the training. The former suggests that the health care workers did not find interdisciplinary approach to be complicated and the time spent on team-based care was worthwhile. It is conceivable that the uncertainty regarding the time requirement for a multidisciplinary patient care plan could change to positive attitudes when the practitioners are actually involved in developing this patient care plan (Kuipers et al., 2021).
Overall, these findings indicate that the participants had a positive attitude toward interdisciplinary teamwork, suggesting that these professionals are likely to embrace interprofessional collaborative practice. As observed in one study by Siongco et al., (2021), health care practitioners are usually exposed to interprofessional practice leading to a better appreciation of the role of team collaboration in achieving work efficiency and improved health outcomes for patients (Siongco et al., 2021). This will result in positive attitudes towards interdisciplinary approach. Interdisciplinary collaboration by health care workers also has implications for the training of health professional students and residents; it affords trainees the opportunity to acquire appropriate interprofessional skills from experienced practitioners (Algahtani et al., 2021).
These competencies are likely to enhance interprofessional collaboration when they graduate as professionals in the future (Spaulding et al., 2021). Since training improves health workers' attitudes towards teamwork, team skills, and behaviour, these observed positive attitudes are likely to be augmented after our interprofessional HIV training. Given the positive attitude of these professionals towards interdisciplinary teamwork, it is probably about time to consider implementing interprofessional education in the pre-service training curriculum of the various health professions and complement this with in-service training for practising professionals.
Consistent with the results of previous studies, we observed that attitudes towards teamwork improved with professional experience; old providers (health professionals who had been working for more than a year) had better attitudes compared to new providers, as were older professionals (> 5 years) compared to younger providers. Older professionals were more likely to have worked longer. The differences observed across facilities and professions could be partly explained by the number of years of professional experience.
In one study in Germany, physicians acquired more interprofessional approach including teamwork through work experience rather than pre-service training, while the converse was true for nurses (Straub et al., 2020). Interprofessional approach has been shown to improve interprofessional competencies including team skills of practicing health professionals (Spaulding et al., 2021).
Our study shows differences between perceptions about the interdisciplinary approach to patient care. In general, physicians perceived that the team had prerequisites needed for teamwork as well as positive teamwork effects. In previous studies, physicians in primary care have been found to be more reluctant to engage in teamwork (El-Awaisi et al., 2021). However, Lunde et al., (2021) show that exposure to teamwork helps professionals to see the meaning of collaboration. According to the Swedish NCHP, nurses and physicians are prescribed to participate in universal team-based visits at four specific ages (Inera et al., 2019), which is in relation to the present finding.
The present results reflect health workers perception toward teamwork within Asaba specialist hospital, possibly being related to the introduced team-based visits, and their new knowledge and experiences related to this. Furthermore, the psychologists did not participate in team-based visits to the same extent as nurses and physicians, which can possibly have influenced their perceptions about the team characteristics. The role and responsibilities of the psychologists in the CHS team might not be sufficiently clear in the NCHP and thus does not match the needs or are not viewed as being relevant from the psychologists’ perspective according to the reasoning by Tell et al. (2019).
The results show that professionals attending to patient were more likely to report all types of investigated teamwork as well as a perception of continuity within the team. The findings correspond with previous studies showing the importance of co-location for enabling teamwork (Gregory et al., 2022).
According to previous definitions groups of professionals working together does not always mean working as a team. Consultations and team meetings were not associated with team prerequisites and team effects to the same extent as team-based visits and teamwork in parental groups. According to Ash & Miller, (2021), consultations and team meetings may be considered as other forms of interprofessional collaboration or as team processes that enable teamwork. This is relation to the present study that expressed that health workers had a good perception interdisciplinary approach to patient care.
Summary of The Study
This study found that health care professionals at the specialist hospital appropriate interdisciplinary approach to patient care. To ensure the integration of care, the authors of this current study recommend that facility management hosts awareness campaigns, regarding the transition from referral to collaboration. Interdisciplinary approach is increasingly employed to treat patients. Satisfaction with the work of the interdisciplinary approach was positive among. The results demonstrate that despite the difference between groups, members of interdisciplinary groups were satisfied with interdisciplinary approach.
Limitations of The Study
Some of the limitations of this study were the non-responsiveness of some of the healthcare workers to the study. As for the essence of qualitative approaches, it should be noted that they are based on specific inferences, which can suppress some important issues not encompassed in the analysis. It is important to note that this is the only study conducted in Asaba. And since not only nurses were interviewed, but also other health professionals, it enhances the research, given the inherent interdisciplinary approach.
Further studies could comprise a larger number of healthcare professionals interviewed, so as to expand the diversity of the organizational culture’s specialist hospitals, perhaps establishing a triangulation of findings with those of the present study. Future studies should include questions about demographics. Consequently, findings should be interpreted with caution.
Conclusion
Health care professionals in Asaba Specialist teaching hospital had a positive attitude towards collaborative practice, which differed significantly by age, facility, health profession cadre, and professional experience. Interventions are required to strengthen in-service interprofessional training for health practitioners, especially early career professionals. Investigating whether these positive team attitudes translate into collaborative health care delivery for patients would be worthwhile.
References
- Algahtani, H., Shirah, B., Bukhari, H., Alkhamisi, H., Ibrahim, B., et al. (2021). Perceptions and Attitudes of Different Healthcare Professionals and Students Toward Interprofessional Education in Saudi Arabia: A Cross-Sectional Survey. Journal of Interprofessional Care, 35(3):476-481.
Publisher | Google Scholor - Ash, L., Miller, C., Zaccagnini, M. E. (2021). Interprofessional Collaboration for Improving Patient and Population Health. The Doctor of Nursing Practice Essentials, 163-196.
Publisher | Google Scholor - Bachynsky, N. (2020). Implications for Policy: The Triple Aim, Quadruple Aim, and Interprofessional Collaboration. In Nursing Forum. 55(1):54-64.
Publisher | Google Scholor - Bogossian, F., New, K., George, K., Barr, N., Dodd, N., et al. (2023). The Implementation of Interprofessional Education: A Scoping Review. Advances in Health Sciences Education, 28(1):243-277.
Publisher | Google Scholor - Dumlao, R. (2023). A Guide to Collaborative Communication for Service-Learning and Community Engagement Partners. Taylor & Francis.
Publisher | Google Scholor - El-Awaisi, A., Awaisu, A., Aboelbaha, S., Abedini, Z., Johnson, J., et al. (2021). Perspectives of Healthcare Professionals Toward Interprofessional Collaboration in Primary Care Settings in A Middle Eastern Country. Journal of Multidisciplinary Healthcare, 363-379.
Publisher | Google Scholor - Gregory, E. F., White, E., Wu, K. K., McPeak, K. E., Fiks, A. G. (2022). Implementing team-based newborn well care: Perspectives of nurses and physicians. Journal of Pediatric Nursing, 65:22-28.
Publisher | Google Scholor - Gyory, J. T., Cagan, J., Kotovsky, K. (2019). Are You Better Off Alone? Mitigating The Underperformance of Engineering Teams During Conceptual Design Through Adaptive Process Management. Research in Engineering Design, 30:85-102.
Publisher | Google Scholor - Inera A.B. (2018). The National Child Health Care Program.
Publisher | Google Scholor - Kelly, R., Mackay, M., Nash, K. L., Cvitanovic, C., Allison, E. H., et al. (2019). Ten Tips for Developing Interdisciplinary Socio-Ecological Researchers. Socio-Ecological Practice Research, 1:149-161.
Publisher | Google Scholor - Kuipers, S. J., Nieboer, A. P., Cramm, J. M. (2021). Making Care More Patient Centered; Experiences of Healthcare Professionals and Patients with Multimorbidity in The Primary Care Setting. BMC Family Practice, 22(1):1-15.
Publisher | Google Scholor - Lunde, L., Moen, A., Jakobsen, R. B., Rosvold, E. O., Brænd, A. M. (2021). Exploring Healthcare Students’ Interprofessional Teamwork in Primary Care Simulation Scenarios: Collaboration to Create a Shared Treatment Plan. BMC Medical Education, 21(1):1-14.
Publisher | Google Scholor - Manyama, T. L., Tshitake, R. M., Moloto, N. B. (2020). The Role of Pharmacists in The Renal Multidisciplinary Team at A Tertiary Hospital in South Africa: Strategies to Increase Participation of Pharmacists. Health SA Gesondheid, 25.
Publisher | Google Scholor - Mheidly, N., Fares, J. (2020). Leveraging Media and Health Communication Strategies to Overcome The COVID-19 Infodemic. Journal of Public Health Policy, 41(4):410-420.
Publisher | Google Scholor - Muthuri, R. N. D. K., Senkubuge, F., Hongoro, C. (2020, June). Determinants of Motivation Among Healthcare Workers in The East African Community Between 2009-2019: A Systematic Review. In Healthcare. 8(2):164.
Publisher | Google Scholor - Onyedibe, K. I., Shehu, N. Y., Pires, D., Isa, S. E., Okolo, M. O., et al. (2020). Assessment of Hand Hygiene Facilities and Staff Compliance in A Large Tertiary Health Care Facility in Northern Nigeria: A Cross-Sectional Study. Antimicrobial Resistance & Infection Control, 9:1-9.
Publisher | Google Scholor - Opele, J. K. (2022). Inter-Professional Collaboration and Knowledge Management Practices Among Clinical Workforce in Federal Tertiary Hospitals in Nigeria. Knowledge Management & E-Learning, 14(3):329-343.
Publisher | Google Scholor - Sibbald, S. L., Misra, V., DaSilva, M., Licskai, C. (2022). A Framework to Support the Progressive Implementation of Integrated Team-Based Care for The Management Of COPD: A Collective Case Study. BMC Health Services Research, 22(1):1-11.
Publisher | Google Scholor - Singh, G. K., Davidson, P. M., Macdonald, P. S., Newton, P. J. (2019). The Perspectives of Health Care Professionals on Providing End of Life Care and Palliative Care for Patients with Chronic Heart Failure: An Integrative Review. Heart, Lung and Circulation, 28(4):539-552.
Publisher | Google Scholor - Siongco, K.L.L, Nakamura, K, Seino, K, Moncatar, T.J.R.T, Tejero, L.M.S, et al. (2019). Improving Community Health Workers’ Attitudes Toward Collaborative Practice in The Care of Older Adults: An In-Service Training Intervention Trial in The Philippines. Int J Environ Res Public Health. 18:9986.
Publisher | Google Scholor - Spaulding, E. M., Marvel, F. A., Jacob, E., Rahman, A., Hansen, B. R., et al. (2021). Interprofessional Education and Collaboration Among Healthcare Students and Professionals: A Systematic Review and Call for Action. Journal of Interprofessional Care, 35(4):612-621.
Publisher | Google Scholor - Spoorthy, M. S., Pratapa, S. K., Mahant, S. (2020). Mental Health Problems Faced by Healthcare Workers Due to The COVID-19 Pandemic-A Review. Asian Journal of Psychiatry, 51:102119.
Publisher | Google Scholor - Straub, C, Heinzmann, A, Krueger, M, Bode, S.F.N. (2020). Nursing Staffs and Physicians’ Acquisition of Competences and Attitudes to Interprofessional Education and Interprofessional Collaboration in Pediatrics. BMC Med Educ. 20:213.
Publisher | Google Scholor - Tell J, Andersson G, Sanmartin Berglund J, Olander E, Anderberg P. (2019). Implementation and Use of Web-Based National Guidelines in Child Healthcare. Karlskrona: Blekinge Tekniska Högskola.
Publisher | Google Scholor