Research Article
Integration of Artificial Intelligence (AI] in Modern Epidemiology: Promise, Risk and Responsibility
- Muhammad Ajmal Dina ID 1*
- Asif Hanif ID 2
- Asifa Karamat ID 4
- Muhammad Shakeel Basit ID 4
- Muhammad Akram Bhutta ID 5
- Anam Arshed ID 3
1 Department of Biostatistics and Epidemiology, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
2 Department of Biostatistics, Faculty of medicine, Sakarya University, Sakarya-Türkiye.
3 Rahbar Medical and Dental College, Lahore Pakistan.
4 Al Aleem Medical College, Gulab Devi Hospital, Lahore Pakistan.
5 Quaid-e-Azam Medical College, Bahawalpur city, Bahawal Victoria Hospital Bahawalpur, Pakistan.
*Corresponding Author: Muhammad Ajmal Dina, Department of Biostatistics and Epidemiology, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.
Citation: Muhammad A. Dina, Hanif A., Arshed A., Karamat A., Muhammad S. Basit, et al. (2026). A Nation in the Grip of Dengue: How Climate, Pollution, and Urbanization Are Feeding a Relentless Killer-The Mosquito, Journal of BioMed Research and Reports, BioRes Scientia Publishers. 10(1):1-11. DOI: 10.59657/2837-4681.brs.26.221
Copyright: © 2026 Muhammad Ajmal Dina, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: November 17, 2025 | Accepted: December 10, 2025 | Published: January 02, 2026
Abstract
Artificial Intelligence (AI) is transforming modern epidemiology with facilitating swift, accurate and extensive analysis of intricate health data. Through sophisticated machine learning techniques and data integration, AI identifies patterns, predicts disease outbreaks and enhances diagnostic precision beyond the capabilities of traditional analytical methods. Its uses encompassing real-time monitoring, risk evaluation and resource distribution are revolutionizing strategies for disease prevention and management. This technological advancement brings significant ethical and governance dilemmas. Issues regarding data privacy, algorithmic bias, and the transparency of models underscore the necessity for strong ethical frameworks and explainable AI (XAI) systems to guarantee fairness and accountability.
This article consolidates recent progress and challenges, suggesting a governance-focused approach that reconciles innovation with ethical obligations. The promoting interdisciplinary collaboration among data scientists, epidemiologists and ethicists, AI can transition from a formidable analytical instrument to a responsible ally in public health. When executed with transparency and inclusivity, AI has the potential to create smarter, more equitable and resilient global health systems.
Keywords: artificial intelligence (AI); epidemiology; machine learning; ethical challenges; public health
Introduction
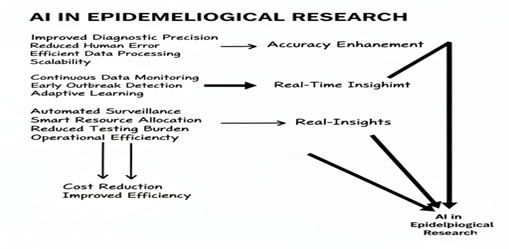
AI is transforming the procedures employed by researchers in the investigation of diseases and public health trends [1]. In epidemiology, it enables scientists to handle and scrutinize extensive health data sets with greater efficiency compared to conventional techniques[2]. The application of algorithms and machine learning, AI is capable of recognizing patterns, forecasting the dissemination of diseases and pinpointing critical risk factors that affect health outcomes[3]. These instruments assist researchers in comprehending intricate interactions among genetics, environment and lifestyle, resulting in more precise conclusions and expedited reactions to health challenges. An overview of how AI supports epidemiological processes is shown in Figure 1.
Figure 1: Figure 1 illustrates the basic understanding of AI in epidemiology.
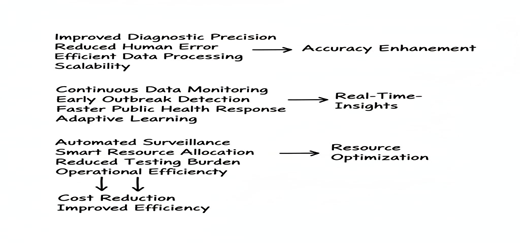
Artificial Intelligence is enhancing various facets of epidemiology as illustrated in Figure 2 of epidemiological practice, including disease surveillance, diagnosis and preventive measures[4].
Figure 2: Advantages of AI in epidemiology and care management
It has the capability to integrate data from hospitals, laboratories and digital health platforms to detect emerging outbreaks and facilitate prompt interventions[5]. The application of AI in research brings forth significant issues related to privacy, bias and the accuracy of data. It is essential to tackle these challenges through transparent and ethical methodologies to guarantee the secure and effective implementation of AI in public health [6]. When utilized judiciously, AI possesses substantial potential to bolster disease management and enhance global population health.
This assists researchers in forecasting outbreaks, monitoring transmission trends and formulating more efficient control strategies[3]. The literature review is segmented into three sections the application of AI in epidemiological studies, its advantages and the potential risks linked to its use. Each segment emphasizes recent discoveries and practical illustrations that demonstrate both the capabilities and the constraints of AI. Grasping these elements offers a comprehensive perspective on how AI can enhance epidemiological research while promoting ethical and transparent practices. This methodology fosters the creation of more intelligent, evidence-driven public health strategies for the future.
Artificial intelligence in disease surveillance
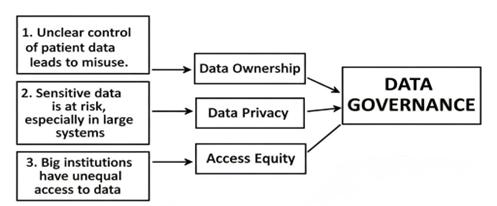
Artificial Intelligence (AI) is increasingly recognized as a vital element in contemporary epidemiology, enhancing the precision of data, operational efficiency and the forecasting of diseases[3]. In the realm of public health surveillance, AI tools, including natural language processing and deep learning, swiftly analyze data from medical records, online platforms and laboratory results to detect initial indicators of outbreaks [7]. Applications of machine learning facilitate the monitoring of disease trends and the prediction of potential risks by charting spatial and temporal patterns. In figure 3 Uncertainties surrounding data ownership and control may result in misuse and privacy threats, especially in extensive healthcare systems. This situation poses a considerable challenge for data governance, given that prominent institutions frequently possess unequal access to information. Consequently, the primary objective is to harmonize strong data privacy with fair access for everyone.
Figure 3: Data and artificial intelligence
Through sophisticated data analysis, artificial intelligence aids in uncovering intricate relationships among genetic, environmental and behavioral elements that affect the progression of diseases[8]. AI-driven diagnostic systems enhance the accuracy of medical imaging and symptom evaluation, resulting in faster and more dependable clinical judgments[9]. Additionally automated data management elevates the quality and uniformity of research databases, minimizing the occurrence of manual errors.
Recent advancements in causal modeling empower researchers to investigate cause and effect dynamics with increased assurance, thereby reinforcing the scientific foundation of epidemiological research. As artificial intelligence continues to evolve, its amalgamation with traditional research methodologies presents new opportunities for developing precise, timely and evidence-based public health initiatives.
Risk and benefits of AI in epidemiological research
Artificial Intelligence (AI) has revolutionized epidemiological research with enhancing accuracy, speed, and responsiveness to public health issues[3]. Advanced algorithms are now capable of identifying subtle patterns within extensive datasets, facilitating the early detection of diseases and providing more dependable predictions. Ongoing analysis of health records, laboratory data and online information aids in real-time outbreak tracking and promotes the effective allocation of medical resources[10]. These advancements also bring forth ethical and technical dilemmas. Concerns regarding data privacy, security vulnerabilities and biases in algorithmic decision-making necessitate thorough scrutiny. Bellow in Table 1 comparison of the benefits and risks of AI in epidemiological research.
Table 1: Comparison of the Benefits and Risks of AI in Epidemiological Research
| Aspect | Benefits of AI in Epidemiology | Associated Risks | References |
| Disease Surveillance & Early Detection | AI enables real-time disease monitoring using data from hospitals, labs, and social media, helping detect outbreaks earlier than traditional methods. | Risk of false alerts or missed signals if the data are incomplete or biased; surveillance systems may overfit to certain regions or populations. | Chadwick, F.Glob J Med Biomed Case Rep 2025 Issue 010, [11] |
| Prediction & Forecasting | Machine learning [ML] models can predict disease spread, case counts, and mortality with high speed and accuracy. | Models may lose accuracy when applied to new data [poor generalization]; overreliance on AI forecasts may mislead policy decisions. | Towfek, S. & Elkanzi, M. Metaheuristic Optimiz. Rev 2024 Issue 1 Pages 14-27 [12] |
| Risk Factor Identification | AI uncovers hidden associations between environmental, genetic, and behavioral factors and disease outcomes. | Spurious or non-causal correlations can be mistaken for true associations without proper epidemiological validation. | Amjad, S., Liaqat, I., Amjad, Z., Fatima, S., Hashmi, M., Khan, W. & Nasir, M.Complementary and Alternative Medicine: Non–Conventional 2024 [13] |
| Data Integration & Management | AI can merge diverse datasets [EHRs, genomics, mobility, climate] for holistic analysis, improving epidemiologic insight. | Combining datasets may increase privacy risks and data leakage; inconsistent standards hinder interoperability. | Suura, S.R. 2025 [14] |
| Diagnosis & Case Classification | AI tools assist in classifying diseases from imaging, text, or wearable data, enhancing diagnostic precision in surveillance studies. | Biased or non-transparent algorithms can misclassify cases, especially in underrepresented populations. | Srinivasan, S.M. & Sharma, V. AI in Disease Detection: Advancements and Applications 2025 Pages 123-146 [15] |
| Resource Allocation & Decision Support | AI predicts high-risk areas or populations, helping allocate vaccines, ICU beds, or public health interventions efficiently. | Overreliance may ignore local context or social determinants not captured in the data. | Ali, H. Int J Res Publ Rev 2024 Issue 8 Pages 4605-19 [4] |
| Speed & Scale of Analysis | AI processes massive datasets rapidly, reducing analysis time and enabling real-time dashboards for policymakers. | Automation may amplify data errors; poor-quality input data can lead to misleading conclusions (“garbage in, garbage out”). | Vegineni, G.C. & Marella, B.C.C. AI-Enabled Sustainable Innovations in Education and Business 2025 Pages 251-276 [16] |
The restricted transparency associated with AI decision-making, frequently referred to as the black-box issue, complicates the evaluation of reliability and fairness. Tackle these obstacles, it is essential for researchers to guarantee that AI systems are transparent, ethically oriented and founded on a variety of high-quality data[6, 17]. Establishing explicit policies and accountability frameworks will be vital for the responsible and effective incorporation of AI into epidemiological research.
AI Applications in Epidemiology
The incorporation of AI into epidemiological research has profoundly altered the methods of collecting, processing and interpreting public health data. The merging sophisticated computational techniques with conventional analytical practices, AI has transitioned epidemiology from a reactive stance to one focused on proactive prediction and prevention[3]. Automated data processing and intelligent pattern recognition facilitate quicker outbreak detection, precise identification of risk factors and enhanced diagnostic accuracy[18]. These advancements empower researchers and policymakers to make prompt, evidence-based decisions that improve population health outcomes.
Real-time outbreak detection with AI
Artificial Intelligence (AI) has emerged as a crucial element in contemporary disease surveillance, transforming conventional monitoring systems into real-time, predictive methodologies[19]. Machine learning technologies scrutinize data sourced from social media, online conversations and digital news outlets to identify atypical activities that may signal the onset of new outbreaks[20]. The analysis of Electronic Health Records (HER) aids in recognizing abrupt surges in symptoms or hospital admissions, facilitating quicker identification of potential epidemics.
Deep learning and time-series forecasting techniques are employed to anticipate the spread of infectious diseases, thereby enhancing timely public health strategies. Geospatial AI methodologies generate hotspot maps that pinpoint clusters and areas of transmission, informing targeted containment efforts[21]. Natural Language Processing [NLP] plays a significant role by extracting syndromic data from unstructured clinical documentation[22]. These AI-driven approaches enhance the accuracy, responsiveness and scalability of surveillance systems, equipping health authorities with dependable information for prompt intervention and effective disease management.
AI in disease risk assessment
Artificial Intelligence (AI) is crucial in identifying risk factors for diseases with analyzing extensive and intricate datasets that surpass the capabilities of conventional statistical techniques. Machine learning facilitates exposure mapping with examining environmental, occupational and lifestyle factors to reveal their collective impact on the progression of diseases[23]. AI-driven genomic analysis identifies associations between genetic or epigenetic variations and susceptibility to diseases, thereby enhancing the precision of risk predictions[14]. Integrating multi-omics data, AI synthesizes various biological information, including genomics, proteomics and metabolomics to create a holistic view of disease mechanisms.
Outcome modeling based on deep learning further investigates non-linear interactions between exposures and health outcomes, resulting in more accurate risk assessments[24]. Unsupervised learning methods improve this approach by uncovering hidden clusters and subtle differences in disease susceptibility at the population level[8]. These AI-enhanced techniques bolster causal inference, advance precision epidemiology and aid in the formulation of targeted prevention and intervention strategies.
AI-driven patient management
AI technologies are becoming increasingly essential in enhancing clinical decision-making through improved diagnostic accuracy, efficiency and personalized care[25]. In the realm of medical imaging, deep learning models, particularly convolutional neural networks (CNNs) are proficient in interpreting X-rays[26], CT scans and MRIs, frequently achieving or exceeding the performance levels of experts[27]. Natural language processing (NLP) systems play a crucial role in extracting significant information from unstructured electronic health records (EHRs) and clinical notes[22], transforming it into structured data that facilitates quicker and more reliable diagnoses. AI-driven clinical decision support systems (CDSS) merge patient information with medical guidelines to propose customized treatment alternatives, thereby fostering evidence-based healthcare[28]. Triage algorithms aid healthcare professionals in prioritizing patients according to the severity of their conditions, thereby enhancing resource distribution in high-demand clinical or emergency settings[29]. Conversational AI tools like chatbots, improve accessibility by performing initial screenings and assisting with follow-up care. Together, these AI innovations are revolutionizing diagnostic precision, patient management, and the overall effectiveness of healthcare delivery.
AI in health data management
The swift growth and escalating intricacy of health data necessitate effective and intelligent management solutions, which are proficiently offered with AI[30]. Automated data cleansing systems execute crucial preprocessing functions, error identification, normalization and standardization, thereby ensuring the generation of more precise and dependable datasets for analysis[31]. AI-driven source integration amalgamates data from wearable devices, electronic health records (EHRs), laboratory databases and public health registries into cohesive analytical platforms[32]. Sophisticated imputation models predict missing data points, reducing bias and enhancing the quality of predictive modeling.
Real-time dashboards, powered by AI, produce dynamic visual representations that improve situational awareness and inform evidence-based public health decisions[33]. AI-enabled literature mining automates the extraction and synthesis of scientific research, facilitating systematic reviews and the formulation of clinical guidelines, these technologies enhance data accuracy, optimize analysis and bolster the overall efficacy of epidemiological research and health policy development.
Enhancing epidemiological causality
AI is increasingly recognized as an essential instrument for the identification and validation of causal relationships which are fundamental to epidemiological studies[34]. Causal discovery algorithms leverage extensive observational datasets to construct causal graphs, uncovering concealed connections and mechanisms that may elude traditional methodologies. Counterfactual analysis allows researchers to investigate hypothetical "what-if" scenarios, estimating the results of interventions that were not directly observed [35]. Hybrid inference methods merge machine learning with traditional statistical models, combining robust predictive capabilities with enhanced interpretability to improve causal reasoning.
In the realms of social and economic epidemiology, AI-enhanced instrumental estimation aids in the identification of appropriate instruments for quasi-experimental analysis, thereby increasing the precision of causal estimates [36]. Additionally robust simulation techniques rigorously evaluate causal models across various conditions, ensuring their consistency and dependability. Collectively, these AI-driven methodologies propel causal inference in epidemiology forward, offering more compelling evidence for effective, data-informed public health decision-making.
Optimizing epidemiological practice
The incorporation of AI into epidemiological research offers considerable benefits across various domains of public health [24]. AI improves diagnostic accuracy, facilitating earlier and more precise disease identification. It enhances surveillance systems with enabling real-time monitoring and swift detection of new outbreaks, which allows for timely public health interventions, with automating routine tasks and optimizing data processing, AI boosts efficiency in both research and healthcare operations[18]. The insights derived from AI promote evidence-based decision-making and a more effective allocation of scarce health resources, these advantages enhance the accuracy, promptness and overall efficacy of epidemiological practices, leading to more agile and informed public health strategies.
Reducing human error with AI
AI presents numerous significant benefits in the field of epidemiology, beginning with enhanced accuracy[3]. The statistical approaches often face limitations when it comes to analyzing extensive, intricate and high-dimensional datasets. In contrast, machine learning and deep learning algorithms possess the ability to uncover subtle, nonlinear patterns those traditional methods might overlook[37]. This proficiency improves diagnostic accuracy, especially in domains like medical imaging and genomic analysis. AI diminishes human error with reducing subjective biases and inconsistencies in the interpretation of data. In addition to accuracy, AI offers exceptional efficiency, enabling the rapid processing of large datasets and converting raw data into actionable insights[3]. Its scalability facilitates deployment across national or global surveillance systems without a corresponding increase in human resources, rendering it particularly advantageous in settings with limited resources.
Another significant benefit of AI is its capacity to deliver real-time insights, transforming public health practices from reactive monitoring to proactive intervention. Unlike traditional surveillance systems that depend on periodic or retrospective reporting, AI continuously evaluates various data sources, such as electronic health records, social media and mobile health applications[38]. This ongoing monitoring allows for the early detection of outbreaks, as algorithms swiftly recognize unusual trends or anomalies that could signify emerging threats. Prompt alerts enable timely public health responses, including targeted testing, vaccination initiatives or mobility restrictions[39]. AI’s adaptive learning capabilities permit models to revise predictions as new data becomes available, ensuring accuracy and relevance in ever-changing epidemiological contexts.
AI for resource optimization
Artificial Intelligence is essential for optimizing resources in public health systems which frequently encounter constraints in funding and staffing. Automated surveillance diminishes the dependence on labor-intensive manual processes, thereby reducing operational expenses and enhancing overall efficiency [40]. AI-driven allocation models assist in directing vaccines, diagnostic kits, and healthcare personnel to populations at high risk, ensuring the greatest impact while reducing waste. In clinical environments, risk-based testing gives priority to individuals who are most likely to be affected, thus avoiding unnecessary procedures and concentrating resources where they are most required. AI facilitates the integration, harmonization and analysis of data, functions that have traditionally demanded significant human effort[24]. These applications conserve time and resources, enabling public health professionals to concentrate on strategic planning and intricate decision-making.
Ethical challenges of AI in epidemiology
AI possesses the capacity to revolutionize epidemiology, it simultaneously introduces significant ethical and practical dilemmas[3]. Major issues encompass data governance, transparency of models, algorithmic bias and the necessity of informed consent, all of which can influence public confidence, the integrity of research and equity in health outcomes. Neglecting to tackle these concerns could undermine the precision of insights generated with AI and worsen pre-existing inequalities in healthcare access and quality[41]. It is crucial to identify and alleviate these risks to guarantee the responsible and fair use of AI in epidemiological studies.
Data ownership and privacy challenges
One significant obstacle in the integration of AI within epidemiology is the issue of data ownership and control[24]. AI technologies require access to extensive, sensitive datasets which encompass personal health records, social media interactions and mobile tracking data[42]. This dependency gives rise to considerable privacy issues, particularly when data is gathered without clear consent or is inadequately anonymized. The uncertainty regarding data ownership whether it lies with patients, healthcare organizations, governments tech companies further complicate governance and accountability[43]. Differences in data access may lead to power imbalances, benefiting well-funded entities but marginalizing underrepresented groups from the advantages of AI-enhanced public health initiatives[44]. Tackling these challenges is essential to guarantee the ethical, fair and transparent application of AI in epidemiology.
Another significant challenge pertains to model transparency and interpretability. Numerous sophisticated machine learning models, especially deep learning frameworks, function as black boxes, generating predictions without elucidating the rationale behind them. In the field of epidemiology, where AI-generated outputs can influence public health policies and clinical protocols, this lack of transparency erodes trust and complicates expert evaluation and validation. Explainable AI [XAI] methodologies seek to enhance interpretability but their implementation is still limited and many existing tools fail to provide actionable insights for healthcare professionals or public health authorities[45]. This lack of clarity raises ethical and legal dilemmas, particularly when AI is involved in critical decisions such as outbreak management, resource distribution, or patient prioritization, underscoring the pressing need for transparent and accountable AI frameworks.
Ethical and risk considerations of AI in epidemiology
Algorithmic bias poses a considerable obstacle in AI-driven epidemiology, as models are influenced by the data utilized for training[3]. Historical and structural inequities associated with race, gender, geography or socioeconomic status can become ingrained in datasets, resulting in AI systems that replicate or even exacerbate these disparities[46]. In the realm of public health, biased algorithms may produce unequal risk assessments, underdiagnose conditions within minority groups, or misallocate healthcare resources[47]. For example, a model predominantly trained on urban hospital data may yield suboptimal results in rural or underserved areas, thereby worsening existing health disparities. Tackling these biases necessitates technical strategies like fairness audits and bias-correction metrics, in conjunction with interdisciplinary oversight from ethicists[48], epidemiologists and representatives from affected communities to guarantee responsible and equitable deployment of AI.
Informed consent represents another intricate challenge in AI-based epidemiology. Conventional consent models frequently prove inadequate when data is reused across various studies or amalgamated with external datasets for secondary analysis. The characteristics of AI systems further hinder participants' comprehension of how their data will be utilized, raising questions about the ethical legitimacy of consent[49]. These issues are particularly pressing in public health surveillance, Innovative solutions, such as dynamic consent and community-based consent frameworks, seek to tackle these difficulties, although their implementation remains inconsistent and resource-demanding.
Loop-oriented framework for AI applications in epidemiology
The Loop-Oriented framework in AI epidemiology classifies applications based on their direct outputs, referred to as "loops," which include early warning, pattern recognition and treatment guidance[50]. Geospatial AI that generates hotspot identification loops plays a crucial role in disease surveillance, whereas reinforcement learning that produces adaptive treatment loops enhances clinical decision-making.
Aligning operational objectives like real-time monitoring or high-risk population detection with loops ensures that investments are directed towards tools that yield the most significant public health benefits[51]. Context is essential low- and middle-income countries might prioritize cost-effective surveillance and dashboards, while high-income regions may concentrate on personalized therapeutics and policy modeling. The framework fosters collaboration among AI developers, epidemiologists, and policymakers, thereby enhancing usability and facilitating ethical oversight[51]. Loops that necessitate human supervision, like clinical diagnosis, are differentiated from automated processes such as signal detection. The Overloop framework builds upon this idea, illustrating how outputs from one AI domain can enhance others.
The detection of outbreaks can initiate risk factor analyses, while diagnostic information can refine population-level causal models. Integrated systems that connect surveillance, risk mapping, and treatment evaluation amplify benefits, enabling precise simulations and ongoing learning[42]. Creating AI with overloop potential promotes the establishment of shared data pipelines, cross-domain validation, and scalable, adaptive epidemiological systems. These frameworks inform research and policy by highlighting multi-domain impacts, thereby enhancing outbreak response, risk mitigation, and overall public health decision-making.
AI risk loops in epidemiology
Artificial intelligence has emerged as a significant asset in the field of epidemiology, providing novel avenues for disease monitoring, diagnosis and causal analysis each application entails particular ethical, technical and operational challenges that necessitate careful oversight[52]. In the realm of disease surveillance and outbreak forecasting, AI technologies such as social media analytics and spatial hotspot mapping are heavily reliant on personal and locational data[53]. This reliance prompts concerns regarding privacy, consent, and the potential for algorithmic bias. Underrepresented vulnerable populations may exacerbate existing health inequalities. To mitigate these challenges, it is crucial to enforce robust data protection protocols, perform audits to guarantee demographic inclusivity, and establish transparent processes for acquiring informed consent during data gathering with proactively addressing these risks, AI can be effectively incorporated into public health initiatives without undermining ethical or social principles, in table 2 a detailed AI risk loop, mapping cross-domain risks and ethical challenges in epidemiological applications.
Table 2: AI Risk loop table: Mapping cross-domain risks and ethical challenges in epidemiological applications
| Epidemiological Domain | AI-specific risks | Ethical & methodological challenges | Mitigation Strategies |
| Disease surveillance, outbreak prediction | Data Privacy breaches; algorithmic bias in detection | Transparency, accountability, ownership of public health data | Develop secure AI architectures; apply privacy-preserving federated learning; establish data governance frameworks [54] |
| Risk Factor Identification | Incomplete or skewed datasets; feature misinterpretation | Interpretability of AI models; risk of misclassification | Use explainable AI [XAI] tools; integrate domain expert validation. [55] |
| Diagnosis & Treatment | Clinical Bias; Opaque Decision-Making Models | Model Explain ability; Health Equity and Disparity Bias | Implement interpretable diagnostic models; continuous bias auditing and retraining, [56] |
| Data Management & Analysis | Overfitting and Poor Generalization; Automation Bias | Informed Consent and Data Reuse Ethics | Standardize consent processes; enhance human-in-the-loop validation. [57] |
| Causal Inference and Simulation | Black Box Causality; Ethical Risks in Predictive Simulation | Instrumental Validity; Accountability in Synthetic Modeling | Use causal inference frameworks; perform scenario-based ethical testing. [58] |
In the process of identifying risk factors, AI technologies such as genomic linking and multi-omics integration manage highly sensitive data, which poses a risk of misuse. Models that are trained on incomplete or historical datasets may inadvertently perpetuate societal biases, resulting in erroneous conclusions regarding vulnerable populations[59].
In the realms of diagnosis and treatment, AI frequently operates as a black-box decision-maker, potentially diminishing clinician confidence, generating legal ambiguities, and eroding patient trust. The automated systems analyze medical images or clinical histories without providing clear rationales to mitigate these issues, it is essential for models to be transparent, permit clinician oversight, and incorporate patient education to uphold informed trust. The data management and analysis introduce challenges, such as disputes over ownership, the potential for automated error propagation, and varying standards for metadata[60]. The integration of diverse datasets without explicit accountability can lead to both ethical and operational uncertainties, underscoring the necessity for meticulous governance and strong data protocols.
Conclusion
This study explores how Artificial Intelligence is transforming the domain of epidemiology with examining its key applications, benefits, and potential risks. AI empowers researchers to analyze large datasets, reveal hidden patterns and make swift, evidence-based decisions that aim to improve population health. However, its use also brings forth ethical and technical challenges that require careful management. To address these issues the study proposes three approaches: creating feedback systems to ensure AI technologies align with specific epidemiological goals, encouraging interdisciplinary collaboration to enhance data use and disease prediction, and recognizing risks to ensure fairness and transparency. These approaches facilitate the responsible, efficient and ethical use of AI in public health research and practice.
Abbreviations
AI – Artificial Intelligence
ML – Machine Learning
EHR – Electronic Health Record
NLP – Natural Language Processing
XAI – Explainable Artificial Intelligence
CDSS – Clinical Decision Support System
WHO – World Health Organization
PHI – Public Health Informatics
Declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Data Availability
Not applicable.
Competing interests
The authors declare no competing interests.
Funding
No funding supported received by anyone.
Authors contributions
M.A.D., A.H., A.A. were involved in conceptualization, editing, and original manuscript writing, A.K., M.B., M.S.B., M.A.B. were in language, language editing, all authors approved the final version of the manuscript.
References
- Rashid, Z., Ahmed, H., Nadeem, N., Zafar, S. B., & Yousaf, M. Z. (2025). The paradigm of digital health: AI applications and transformative trends. Neural Computing and Applications, 1–32.
Publisher | Google Scholor - Rahman, S. Z., Senthil, R., Ramalingam, V., & Gopal, R. (2023). Predicting infectious disease outbreaks with machine learning and epidemiological data. Journal of Advanced Zoology, 44(S4):110–121.
Publisher | Google Scholor - Gawande, M. S., Zade, N., Kumar, P., Gundewar, S., Weerarathna, I. N., & Verma, P. (2025). The role of artificial intelligence in pandemic responses: From epidemiological modeling to vaccine development. Molecular Biomedicine, 6(1):1.
Publisher | Google Scholor - Ali, H. (2024). AI for pandemic preparedness and infectious disease surveillance: Predicting outbreaks, modeling transmission, and optimizing public health interventions. International Journal of Research Publication and Reviews, 5(8):4605–4619.
Publisher | Google Scholor - Miglietta, L., Rawson, T. M., Galiwango, R., Tasker, A., Ming, D. K., Akogo, D., et al. (2025). Artificial intelligence and infectious disease diagnostics: State of the art and future perspectives. The Lancet Infectious Diseases.
Publisher | Google Scholor - Akter, L., Mondal, R. S., & Bhuiyan, M. N. A. (2025). Artificial intelligence application in public health: Advancement and associated challenges. Journal of Primeasia, 6(1):1–10.
Publisher | Google Scholor - Villanueva-Miranda, I., Xiao, G., & Xie, Y. (2025). Artificial intelligence in early warning systems for infectious disease surveillance: A systematic review. Frontiers in Public Health, 13, 1609615.
Publisher | Google Scholor - Kraemer, M. U. G., Tsui, J. L.-H., Chang, S. Y., Lytras, S., Khurana, M. P., Vanderslott, S., et al. (2025). Artificial intelligence for modelling infectious disease epidemics. Nature, 638(8051):623–635.
Publisher | Google Scholor - Hirosawa, T., & Shimizu, T. (2025). A narrative review of artificial intelligence in medical diagnostics. Computers, Materials & Continua, 83(3).
Publisher | Google Scholor - Lawal, O. P., Igwe, E. P., Olosunde, A., Chisom, E. P., Okeh, D. U., Olowookere, A. K., et al. (2025). Integrating real-time data and machine learning in predicting infectious disease outbreaks: Enhancing response strategies in Sub-Saharan Africa. Asian Journal of Microbiology and Biotechnology, 10(1):147–163.
Publisher | Google Scholor - Chadwick, F. (2025). AI for disease surveillance in the modern era: Early detection and rapid response. Global Journal of Medical and Biomedical Case Reports, 1(010).
Publisher | Google Scholor - Towfek, S., & Elkanzi, M. (2024). A review on the role of machine learning in predicting the spread of infectious diseases. Metaheuristic Optimization Review, 2(1):14–27.
Publisher | Google Scholor - Amjad, S., Liaqat, I., Amjad, Z., Fatima, S., Hashmi, M., Khan, W., et al. (2024). Genomic insights: Predicting obesity through AI and machine learning. Complementary and Alternative Medicine: Non-Conventional, 90.
Publisher | Google Scholor - Suura, S. R. (2025). Integrating artificial intelligence, machine learning, and big data with genetic testing and genomic medicine to enable earlier, personalized health interventions. Deep Science Publishing.
Publisher | Google Scholor - Srinivasan, S. M., & Sharma, V. (2025). Applications of AI in cardiovascular disease detection. In AI in disease detection: Advancements and applications (123–146).
Publisher | Google Scholor - Vegineni, G. C., & Marella, B. C. C. (2025). Integrating AI-powered dashboards in state government programs for real-time decision support. In AI-enabled sustainable innovations in education and business (251–276). IGI Global Scientific Publishing.
Publisher | Google Scholor - Sabha, S. U. (2025). Artificial intelligence and omics in health and diseases. In Artificial intelligence in human health and diseases (75–92). Springer.
Publisher | Google Scholor - Srivastava, V., Kumar, R., Wani, M. Y., Robinson, K., & Ahmad, A. (2025). Role of artificial intelligence in early diagnosis and treatment of infectious diseases. Infectious Diseases, 57(1):1–26.
Publisher | Google Scholor - Nwakobe, C. F., Okafor, S., & Ilouno, I. O. (2025). Artificial intelligence-powered predictive modeling for disease surveillance and mitigation. International Journal of Multidisciplinary on Science and Management, 2(1):34–42.
Publisher | Google Scholor - Mahapatra, B., Mishra, S., & Nayyar, A. (2025). Mental health prediction using machine learning and deep learning technology. CRC Press.
Publisher | Google Scholor - Yang, X., Wang, H., & Lu, H. (Eds.). (2025). Hotspots and trends in research on early warning of infectious diseases: A bibliometric analysis using CiteSpace. Healthcare.
Publisher | Google Scholor - Methuku, V. (2025). NLP and AI for public health intelligence: Automating disease surveillance from unstructured data. ICCK Transactions on Emerging Topics in Artificial Intelligence, 2(1):43–56.
Publisher | Google Scholor - Isola, S., Murdaca, G., Brunetto, S., Zumbo, E., Tonacci, A., & Gangemi, S. (2024). The use of artificial intelligence to analyze the exposome in the development of chronic diseases. Informatics.
Publisher | Google Scholor - Chen, S., Yu, J., Chamouni, S., Wang, Y., & Li, Y. (2024). Integrating machine learning and artificial intelligence in life-course epidemiology. BMC Medicine, 22(1):354.
Publisher | Google Scholor - Khalifa, M., Albadawy, M., & Iqbal, U. (2024). Advancing clinical decision support: The role of artificial intelligence across six domains. Computer Methods and Programs in Biomedicine Update, 5, 100142.
Publisher | Google Scholor - Nafisah, S. I., & Muhammad, G. (2024). Tuberculosis detection in chest radiographs using convolutional neural networks and explainable artificial intelligence. Neural Computing and Applications, 36(1):111–131.
Publisher | Google Scholor - Paudyal, R., Shah, A. D., Akin, O., Do, R. K. G., Konar, A. S., Hatzoglou, V., et al. (2023). Artificial intelligence in CT and MR imaging for oncological applications. Cancers, 15(9):2573.
Publisher | Google Scholor - Khude, H., & Shende, P. (2025). AI-driven clinical decision support systems: Revolutionizing medication selection and personalized drug therapy. Advances in Integrative Medicine, 100529.
Publisher | Google Scholor - Da’Costa, A., Teke, J., Origbo, J. E., Osonuga, A., Egbon, E., & Olawade, D. B. (2025). AI-driven triage in emergency departments. International Journal of Medical Informatics, 105838.
Publisher | Google Scholor - Al Sharif, A. M. S., Alqudhaya, A. S., Alqahtani, M. A., Almotiri, G. S., & Albaqami, W. M. (2024). Harnessing big data and artificial intelligence for health crisis management. Journal of International Crisis and Risk Communication Research, 7(S8):906.
Publisher | Google Scholor - Alowais, S. A., Alghamdi, S. S., Alsuhebany, N., Alqahtani, T., Alshaya, A. I., Almohareb, S. N., et al. (2023). Revolutionizing healthcare: The role of artificial intelligence in clinical practice. BMC Medical Education, 23(1):689.
Publisher | Google Scholor - Saikia, T., Acharjee, T., & Bhatia, D. (2025). Data science: Healing with algorithms. Innovation and Emerging Technologies, 12:2530009.
Publisher | Google Scholor - Amanna, A. (2025). Deploying next-generation artificial intelligence ecosystems for real-time biosurveillance, precision health analytics and dynamic intervention planning in life science research.
Publisher | Google Scholor - Matthay, E. C., Neill, D. B., Titus, A. R., Desai, S., Troxel, A. B., Cerda, M., et al. (2025). Integrating artificial intelligence into causal research in epidemiology. Current Epidemiology Reports, 12(1):6.
Publisher | Google Scholor - Olayinka, O. H. (2024). Causal inference and counterfactual reasoning in high-dimensional data analytics for robust decision intelligence. International Journal of Engineering Technology Research and Management.
Publisher | Google Scholor - Shafa, H. (2025). Artificial intelligence-driven business intelligence models for enhancing decision-making in U.S. enterprises. ASRC Procedia: Global Perspectives in Science and Scholarship, 1(01):771–800.
Publisher | Google Scholor - Rane, N. L., Paramesha, M., Choudhary, S. P., & Rane, J. (2024). Machine learning and deep learning for big data analytics: A review of methods and applications. Partners Universal International Innovation Journal, 2(3):172–197.
Publisher | Google Scholor - Vargas-Santiago, M., León-Velasco, D. A., Maldonado-Sifuentes, C. E., & Chanona-Hernandez, L. (2025). A state-of-the-art review of artificial intelligence (AI) applications in healthcare: Advances in diabetes, cancer, epidemiology, and mortality prediction. Computers, 14(4):143.
Publisher | Google Scholor - Taseen, S., Yousafzai, M. T., & Qureshi, M. F. H. (2025). Harnessing artificial intelligence and digital technology for enhancing routine immunization among zero-dose children. Digital Health, 11, 20552076251382086.
Publisher | Google Scholor - Faiyazuddin, M., Rahman, S. J. Q., Anand, G., Siddiqui, R. K., Mehta, R., Khatib, M. N., et al. (2025). The impact of artificial intelligence on healthcare: A comprehensive review of advancements in diagnostics, treatment, and operational efficiency. Health Science Reports, 8(1):e70312.
Publisher | Google Scholor - Dave, E., Folorunsho, A., & Noel, D. (2025). From digital childhoods to predictive health systems: The role of artificial intelligence and multimorbidity research in shaping the future of public health in South Asia.
Publisher | Google Scholor - da Silva Mendes, V. I., Milhomens de Ferreira Mendes, B., Moura, R. P., Mota Lourenço, I., Ferreira Alves Oliveira, M., Lee Ng, K., et al. (2025). Harnessing artificial intelligence for enhanced public health surveillance: A narrative review. Frontiers in Public Health, 13:1601151.
Publisher | Google Scholor - Nogaroli, R. (2025). Ethical and legal aspects of artificial intelligence (AI) in medical service contracts. In Medical liability and artificial intelligence: Brazilian and European legal approaches (123–206). Springer.
Publisher | Google Scholor - Odumbo, O. R. (2025). Explainable AI and federated learning in healthcare supply chain intelligence: Addressing ethical constraints, bias mitigation, and regulatory compliance for global pharmaceutical distribution. International Journal of Computer Applications Technology and Research, 14(4):16–29.
Publisher | Google Scholor - Alghamdi, S., Mehmood, R., Alqurashi, F., & Alzahrani, A. (2025). Paving the roadmap for XAI and IML in healthcare: Data-driven discoveries and the FIXAIH framework. IEEE Access.
Publisher | Google Scholor - Walker, L. (2024). Artificial narrow intelligence-driven diagnostics: Impacts, inequities, and policy imperatives in global healthcare. Technische Universität Wien.
Publisher | Google Scholor - Williams, N. H. (2024). Artificial intelligence and healthcare: The impact of algorithmic bias on health disparities. Springer.
Publisher | Google Scholor - Jones, R. K. (2025). Algorithmic bias and fairness in biomedical and health research. In Ensuring secure and ethical STM research in the AI era (287–324). IGI Global Scientific Publishing.
Publisher | Google Scholor - Youssef, A., Nichol, A. A., Martinez-Martin, N., Larson, D. B., Abramoff, M., Wolf, R. M., et al. (2024). Ethical considerations in the design and conduct of clinical trials of artificial intelligence. JAMA Network Open, 7(9):e2432482.
Publisher | Google Scholor - Muley, A., Cheemalapati, S., & Muzumdar, P. (2025). The role of AI in epidemiological research: Applications, benefits, and risks in modern public health. Asian Journal of Medicine and Health, 23(6):89–107.
Publisher | Google Scholor - Saadatzadeh, R. (2024). The future of public health: Integrating artificial intelligence in disease surveillance and prevention. Journal of Foresight and Health Governance, 1(2):1–15.
Publisher | Google Scholor - Deivayanai, V., Swaminaathanan, P., Vickram, A., Saravanan, A., Bibi, S., Aggarwal, N., et al. (2025). Transforming healthcare: The impact of artificial intelligence on diagnostics, pharmaceuticals, and ethical considerations. International Journal of Surgery, 111(7):4666–4693.
Publisher | Google Scholor - Nwankwo, E. I., Emeihe, E. V., Ajegbile, M. D., Olaboye, J. A., & Maha, C. C. (2024). Artificial intelligence in predictive analytics for epidemic outbreaks in rural populations. International Journal of Life Science Research Archive, 7(1):078–094.
Publisher | Google Scholor - Mohanadas, S. (2025). Next-generation predictive analytics for global disease outbreaks: Bridging innovation, ethics, and impact. European Journal of Computer Science and Information Technology, 13(4):1–23.
Publisher | Google Scholor - Hanna, M. G., Pantanowitz, L., Jackson, B., Palmer, O., Visweswaran, S., Pantanowitz, J., et al. (2025). Ethical and bias considerations in artificial intelligence/machine learning. Modern Pathology, 38(3):100686.
Publisher | Google Scholor - Raza, S., Shaban-Nejad, A., Dolatabadi, E., & Mamiya, H. (2024). Exploring bias and prediction metrics to characterise the fairness of machine learning for equity-centered public health decision-making: A narrative review. IEEE Access.
Publisher | Google Scholor - Tejani, A. S., Ng, Y. S., Xi, Y., & Rayan, J. C. (2024). Understanding and mitigating bias in imaging artificial intelligence. Radiographics, 44(5):e230067.
Publisher | Google Scholor - Kirfel, L., MacCoun, R. J., Icard, T., & Gerstenberg, T. (2025). When AI meets counterfactuals: The ethical implications of counterfactual world simulation models. AI and Ethics, 1–12.
Publisher | Google Scholor - Dhanda, S. S., Panwar, D., Lin, C.-C., Sharma, T. K., Rastogi, D., Bindewari, S., et al. (2025). Advancement in public health through machine learning: A narrative review of opportunities and ethical considerations. Journal of Big Data, 12(1):1–58.
Publisher | Google Scholor - Benjamin, M. (2025). AI-driven frameworks for enhancing data quality in big data ecosystems: Error detection, correction, and metadata integration.
Publisher | Google Scholor