Case Report
Geant Solitary Osteochondroma of Distal Femur Managed with Complete Excision: A Case Report
- Daoudi M *
Department of Traumatology - Orthopedics, Avicenna Military Hospital. Marrakech. Morocco.
*Corresponding Author: Daoudi M, Department of Traumatology - Orthopedics, Avicenna Military Hospital. Marrakech. Morocco.
Citation: Daoudi. M. (2025). Geant Solitary Osteochondroma of Distal Femur Managed with Complete Excision: A Case Report, Clinical Case Reports and Studies, BioRes Scientia Publishers. 11(1):1-3. DOI: 10.59657/2837-2565.brs.25.285
Copyright: © 2025 Daoudi. M, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: October 16, 2025 | Accepted: October 30, 2025 | Published: November 06, 2025
Abstract
Osteochondromas are benign bone tumors that usually occur between the ages of 10 and 30. An osteochondroma or exostosis is a benign bone tumor consisting of a bony outgrowth covered by a cartilage cap that occurs commonly in the metaphysis of long bones (distal femur, proximal tibia, proximal humerus) and pelvis. We describe an unusual case of a osteochondroma affecting the distal fémur of a young boy.
Keywords: osteochondroma; distal femur; complete excision
Introduction
Osteochondromas are the most common benign bone tumors, accounting for 20-50% of benign bone tumors and 9% of all bone tumors [1,2]. The majority are solitary and occur due to sporadic mutations, which is different from multiple osteochondromas which is an autosomal dominant trait [3].
Case Report
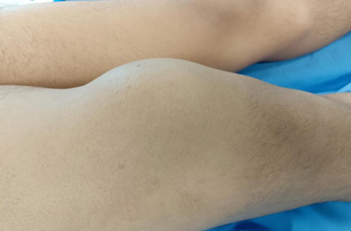
We present the case of 18-year-old young man who consulted us for pain and bone swelling above the Right knee joint, which had persisted for 4 years. At the outset, the swelling presented as compact, painless, and featured a firm osseous texture. associated pain and limitations in knee movement were observed at 90° degrees. Clinical examination revealed an oval-shaped osseous mass originating from the anteromedial aspect of the lower end of the left femur (Figure 1).
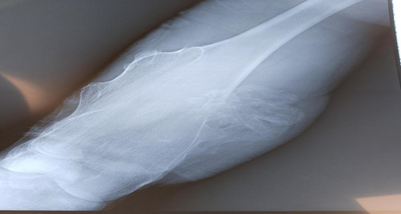
Conventional radiographic images of the left femur, encompassing the knee joint, illustrated a pedunculated osseous mass originating from the anteromedial region of the lower extremity of the left femur. The tumor demonstrated continuous alignment with the femur (Figure 2).
The patient underwent surgery using an anteromedial approach to the distal femur, during which the tumor was exposed and resected end bloc (Figure 3, 4).
Figure 1: Clinical picture of tumour.
Figure 2: Face knee radiographillustrated a pedunculated osseous mass.
Figure 3: Intraoperative picture of Osteochondroma with Perichondrium
Figure 4: Total excision of osteochondroma
Discussion
Osseocartilaginous exostoses are bony protuberances enveloped by a cartilaginous layer, appearing only during the growth period. Although their congenital origin brings them closer to hamartomas, they are categorized as benign bone tumors. Two clinical forms have been identified: solitary exostoses and existing disease [4]. Osteochondromas are frequently observed in adolescents and more rarely in newborns. In the case of solitary exostosis, there is no disparity between the sexes. These tumors show a marked preference for the metaphyseal side of the growth plate, which is in full activity. Frequently, X-rays and CT scans deliver precise diagnostic insights, facilitating the anatomical characterization of the lesion [5]. In imaging, osteochondromas typically present as pedicles or projections resembling sessile bone. Recurrence of exostosis is exceptionally rare and usually occurs when fragments of the cartilage cap remain after excision. For this reason, excision must be performed extraperiosteally. Moreover, recurrence should raise concerns about possible malignant transformation [6.7].
Conclusion
Osteochondromas, prevalent benign bone tumors, usually manifest with cosmetic changes and symptoms arising from mechanical compression of adjacent structures. Any abrupt enlargement associated with pain should raise concerns about potential malignant transformation.
References
- Baklaja R, Pesic MC, Czarnecki J. (2008). Hemostasis and hemorrhagic disorders. Fermentation-Biotec GmbH.
Publisher | Google Scholor - Abdulrahaman, Y., Dallatu, M. K. (2012). Evaluation of prothrombin time and activated partial thromboplastin in patients with diabetes mellitus. Nigerian Journal of Basic and Applied Sciences, 20(1):60-63.
Publisher | Google Scholor - Achneck, H. E., Sileshi, B., Parikh, A., Milano, C. A., Welsby, I. J., et al. (2010). Pathophysiology of bleeding and clotting in the cardiac surgery patient: from vascular endothelium to circulatory assist device surface. Circulation, 122(20):2068-2077.
Publisher | Google Scholor - Thornton P, Douglas J. (2010). Coagulation in pregnancy. Best Practice & Research Clinical Obstetrics & Gynaecology. 24(3):339-352.
Publisher | Google Scholor - Previtali E, Bucciarelli P, Passamonti SM, Martinelli I. (2011). Risk factors for venous and arterial thrombosis. Blood Transfusion. 9(2):120-138
Publisher | Google Scholor - Ochei JO, Kolhatkar AA. (2008). Medical laboratory science: theory and practice. McGraw Hill Education.
Publisher | Google Scholor - Furie, B., Furie, B. C. (2005). Thrombus formation in vivo. The Journal of Clinical Investigation, 115(12):3355-3362.
Publisher | Google Scholor - Madan, R., Gupt, B., Saluja, S., Kansra, U. C., Tripathi, B. K., et al. (2010). Coagulation profile in diabetes and its association with diabetic microvascular complications. The Journal of the Association of Physicians of India, 58:481-484.
Publisher | Google Scholor - Jabeen F, Rizvi HA, Aziz F, Wasti AZ. (2013). Hyperglycemic induced variations in Hematological Indices in Type 2 Diabetics. Int J Adv Res, 1(8):322-334.
Publisher | Google Scholor - McFarlane, I. A. (1997). Endocrine disease and diabetes mellitus. In Williams JC, (Ed), Textbook of Diabetes (2nd Edition) Oxford: Blackwell, 640-660.
Publisher | Google Scholor - Alvin CP. (2001). Diabetes In: principles of internal medicine. 15th ed. New York: MCgraw Hill, 2109-2138.
Publisher | Google Scholor - Soares AL, Sousa MD, Fernandes AP, Carvalho MD. (2010). Hemostatic changes in patients with type 2 diabetes mellitus. Revista Brasileira de Hematologia e Hemoterapia. 32(60):482-488.
Publisher | Google Scholor - Sumitra Dash, RJ Dash. (1995). Levels of natural anticoagulants, antithrombin iii and protein C in diabetes vascular disease. Bahrain Medical Bulletin. 17(4).
Publisher | Google Scholor - Cucuianu, M., Coca, M. (2012). Thrombotic tendency in diabetes mellitus. Revisiting and revising a study initiated 30 years ago. Romanian Journal of Internal Medicine (Revue Roumaine de Medecine Interne), 50(2):107-115.
Publisher | Google Scholor - Sapkota B, Shrestha SK, Poudel S. (2013). Association of activated partial thromboplastin time and fibrinogen level in patients with type II diabetes mellitus. BMC Research Notes. 6:1-5.
Publisher | Google Scholor - Karim F, Akter QS, Jahan S, Khanom A, Haque S, et al. (2015). Coagulation Impairment in Type 2 Diabetes Mellitus. J Bangladesh Soc Physiol. 21;10(1):26-29.
Publisher | Google Scholor - Thukral S, Hussain S, Bhat S, Kaur N, Reddy A. (2018). Prothrombin time (PT) and activated partial thromboplastin time (APTT) in type 2 diabetes mellitus, a case control study. International Journal of Contemporary Medical Research. 5(8):5-9.
Publisher | Google Scholor - Chaitanya PK, Kavuri S, Devi KA. (2014). Comparison of prothrombin time and activated partial thromboplastin time between patients with diabetes mellitus and diabetics with hypertension. Int J Pharm Bio Sci. 5(3):705-709.
Publisher | Google Scholor - Omer IA. (2020). Estimation of prothrombin time, activated partial thromboplastin time and thrombocytes among Sudanese patients with diabetes. GSC Biological and Pharmaceutical Sciences. 10(1):34-38.
Publisher | Google Scholor - Pandya M, Parmar C, Singh M. (2020). Study of prothrombin time and activated partial thromboplastin time in type II diabetes mellitus. International Journal of Clinical and Diagnostic Pathology. 3:173-175.
Publisher | Google Scholor - Abdulla AM, Elmissbah TE, Hamid EM, Altom FO, Faisal M. (2017). Assessment of coagulation process in diabetic patients using prothrombin time and activated thromboplastin time tests. Int. J. of Multidisciplinary and Current research. 5:343-347.
Publisher | Google Scholor - Fadairo JK, Atere AD, Ogidiolu TO, Abiodun OP. (2016). Assessment of some coagulation indices among type II diabetic subjects in a tertiary facility in South West Region, Nigeria. IOSR-JDMS. 15(6):159-163.
Publisher | Google Scholor - Mariappan A, Deepa VS, Nagendran R. (2017). Evaluation of Coagulation Profile in Type-1 Diabetes:A Hospital Based Prospective Study. International Journal of Biotechnology and Biochemistry. 13(1):49-54.
Publisher | Google Scholor - Merghani MM, Hassan FM. (2016). Coagulation Disturbance among Essential Hypertensive and Diabetes Mellitus Type II Patients-Khartoum State. Bangladesh Journal of Medical Science. 15(3):424-429.
Publisher | Google Scholor - Mard-Soltani M, Dayer MR, Ataie G, Moazedi AA, Dayer MS, et al. (2011). Coagulation factors evaluation in NIDDM patients. American Journal of Biochemistry and Molecular Biology. 1(3):244-254.
Publisher | Google Scholor - Fadellala MH, Mahjaf GM, KaramAlgani AO, Hussein HI, Alfarajabi AM, et al. (2022). Evaluation of PT and PTT among diabetes mellitus type 2 patients in Atbara City during March to July 2018. Excellence Journal for Medical Sciences. 3(1).
Publisher | Google Scholor