Review Article
A Systematic Review on Acute Kidney Injury Following Cardiac Surgery: Clinical Outcomes with Preventive Strategies Over the Decades
- Chandana Sree Madala 1
- Mohammed Quader Naseer 2
- Kanakath Sanvi 3
- Krutika Mahendra Gohil 4
- Sinthujaa Velmurugan 5*
- Alisha Lakhani 6
- Kaarvi Khullar 7
- Richard Paul 3
1Narayana Medical College and Hospital, Nellore, Andhra Pradesh, India
2Ayaan Institute of Medical Sciences, Hyderabad, Telangana, India.
3Al Azhar Medical College and Superspeciality Hospital, Kerala, India.
4HBT Medical College and Dr. Rustom Narsi Cooper Municipal General Hospital, Mumbai, India.
5Mahatma Gandhi Medical College and Research Institute, Puducherry, India.
6Shantabaa Medical College, Amreli, Gujarat, India.
7Government Medical College, Gondia, Maharashtra, India.
*Corresponding Author: Sinthujaa Velmurugan, Mahatma Gandhi Medical College and Research Institute, Puducherry, India.
Citation: Madala C. S., Naseer M. Q., Sanvi K., Gohil K. M., Velmurugan S., et al. (2024). A Systematic Review on Acute Kidney Injury Following Cardiac Surgery: Clinical Outcomes with Preventive Strategies Over the Decades, Journal of Clinical Cardiology and Cardiology Research, BioRes Scientia Publishers. 3(2):1-16, DOI: 10.59657/2837-4673.brs.24.033
Copyright: © 2024 Sinthujaa Velmurugan, this is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received: June 11, 2024 | Accepted: July 05, 2024 | Published: July 12, 2024
Abstract
Introduction: Acute kidney injury (AKI) is a common complication following cardiac surgery, contributing to increased morbidity and mortality. This systematic review aims to comprehensively evaluate the incidence, risk factors, and clinical outcomes associated with AKI post-cardiac surgery.
Methods: A systematic search of electronic databases was conducted to identify relevant studies published. Studies reporting on AKI incidence, risk factors, and clinical outcomes in adult patients undergoing cardiac surgery were included. Data were extracted and synthesized following PRISMA guidelines.
Results: A total of 23 studies were included in the review. AKI was associated with increased short and long-term morbidity and mortality, prolonged hospital stays, and higher healthcare costs. Encouraging outcomes were noted when dexmedetomidine, a highly selective α2-adrenergic receptor agonist, was administered during surgery. Two promising non-pharmacological strategies to reduce CSA-AKI are the use of a revolutionary renal guard (RG) system and the introduction of a KDIGO-based treatment bundle. Teprasiran, a new P2Y12 receptor antagonist, was found to significantly reduce the frequency and severity of AKI. The results of this review further highlight the significance of customized preventative measures and risk stratification.
Conclusion: Acute kidney injury is a significant complication following cardiac surgery, with considerable variability in its incidence and associated risk factors. Implementation of preventive strategies is crucial in mitigating AKI-related morbidity and mortality. Further research is warranted to optimize patient outcomes and healthcare resource utilization in this population.
Keywords: acute kidney injury; dexmedetomidine; cardiac surgery; preventive measure
Introduction
Acute Kidney Injury (AKI) is a prevalent and frequently encountered complication following cardiac surgery, presenting a significant challenge to patient recovery and prognosis owing to its association with amplified morbidity, mortality, and prolonged hospital stays. CSA-AKI is characterized by an abrupt worsening in kidney function following cardiac surgery as demonstrated by a reduction in the glomerular filtration rate. These patients often have risk factors for kidney disease, such as diabetes, hypertension, and hypercholesterolemia. In addition, cardiac surgery is a major surgical procedure which may contribute to an increased risk for AKI. Susantitaphong et al reported that CBP-associated AKI was associated with an 8-fold increase in mortality in a subgroup analysis within a global incidence study of AKI, based on results from 23 studies [1]. A recent meta-analysis reported that irrespective of the diverse criteria used to define AKI, its occurrence following cardiac surgery is consistently correlates with a 2-4 times higher likelihood of early mortality among patients [2]. The RIFLE criteria defined AKI by a 25% reduction in GFR (this was equated with a 50% increase in creatinine level or low urine output [3]. The AKIN definition reserved the urine output criterion of the RIFLE definition, dropped the change in GFR per se, and altered the creatinine definition such that a small increase of 0.3 mg/dL also could diagnose AKI. The AKIN definition also reduced the time over which AKI was to be diagnosed from 7 days to 48 hours [4]. The KDIGO definition united RIFLE and AKIN by allowing the relative change of 50% in creatinine level to be over 7 days, whereas absolute change is restricted to 48 hours [5].
The intricate interplay of multifactorial mechanisms, including reduced cardiac output, ischemia-reperfusion injury, renal vasoconstriction, nephrotoxic results like Cardiopulmonary bypass-induced systemic inflammatory response leading to interstitial inflammation and coagulopathy, and patient specific risk factors, contributes to the development of AKI in this setting [6]. Despite advancements in surgical techniques and perioperative care, the incidence of AKI following cardiac procedures remains substantial, impacting patient outcomes, length of hospital stays, and healthcare costs. Studies have reported the risk factors for AKI, for example, female gender, reduced left ventricular function, the presence of congestive heart failure, diabetes, chronic obstructive pulmonary disease, and elevated preoperative serum creatinine [7]. A meta-analysis of 307 studies involving 1200 patients, reported that plasma NGAL (pNGAL) can be considered to be a sensitive and specific early marker of AKI and can be detected up to 48 h before a diagnostic rise in serum creatinine [8]. Greenwood et al reported that pulse wave velocity, a non-invasive measurement tool to assess arterial stiffness, has been shown to predict kidney disease progression, and cardiovascular and all-cause mortality in patients with chronic kidney disease [9].
CSA-AKI increases the risk of death during admission, which can increase to 50% when there is a need for RRT. In 2017, Legouis D et al. studied a cohort of 4,791 patients and found that the risk of CKD was higher in patients who had experienced CSA-AKI than in the AKI-free population [10]. In the absence of precise biomarkers, it seems that even a mild instance of AKI can lead to a poorer prognosis concerning the likelihood of developing CKD and long-term survival in patients. Therefore, it might be more beneficial to prevent, and detect AKI risks rather than focusing solely on a cure. This becomes especially crucial when taking into account the 2009 NCEPOD, which reported that 30% of cases of AKI were preventable and identified a deficiency of care in 50% of cases [11]. Despite published studies detailing the link of CBP-associated AKI and unfavorable outcomes, there have been few attempts to systematically summarize the prognostic consequences of AKI. This review aims to explore the multifactorial etiology, risk factors, and preventive strategies associated with AKI post-cardiac surgery. Understanding these intricate facets is vital in developing targeted interventions to mitigate the incidence of AKI, ultimately benefitting patient care and reducing the load on healthcare systems.
Methodology
This Comparative study was performed in accordance with published guidelines for systematic review, analysis, and reporting for meta-analysis of Observational studies.
Literature Search Strategy
A comprehensive search was done by the investigators in PubMed, Google Scholar and Scopus using appropriate subject headings and keywords. After an extensive search process, studies from all over the world focusing on Preventive Strategies of AKI and their outcomes were selected. The reference lists of included studies and relevant reviews were manually searched to avoid missing relevant studies. All identified articles were systematically assessed using the inclusion and exclusion criteria. All the selected studies were carefully reviewed once again individually by the team of investigators and then 23 studies matching inclusion criteria were shortlisted for the final comparison. Investigators independently reviewed the retrieved articles and evaluated the quality assessment. All data regarding the articles retrieved were entered into Excel software.
Inclusion and Exclusion Criteria
Various articles related to Acute Kidney Injury following Cardiac Surgery were searched through PubMed, Google Scholar, and Scopus. Studies concentrating on preventive strategies of Acute Kidney Injury (AKI) were shortlisted.
The following articles were excluded from the study: 1) Abstracts 2) Studies in non-English Language Literature 3) Animal studies 4) Studies published before 2000. All other standard studies in English Literature dated from 2000 to 2023 were included. All analyses were based on previously published studies; thus, no ethical approval and patient consent are required. The reviewers performed independent manual screening of all the articles by firstly the titles/abstracts and secondly the full texts. Besides, other relevant literature and references of the included studies were also manually screened.
Data Extraction
Four independent review authors extracted relevant study characteristics and outcomes from the 23 included studies using a standardized and piloted data extraction form. The information collected from each study included: Name of the Study, Author details, Citation, year of Publication, Study design, Methodology used, Results, Preventive strategy used, Conclusion and Limitations of the study. The collected data were thoroughly reviewed again, and the information was cross verified again to prevent any mistakes during data processing. All the collected data were pooled together and the preventive strategies of AKI from all the studies were analyzed and reviewed.
Quality Assessment
Two independent reviewers assessed study quality according to criteria outlined by Downs and Black using the 27-point checklist included within 5 main sections.
The five sections include questions about:
1. Reporting (10 items);
2. External validity (3 items);
3. In- ternal validity/Bias (7 items);
4. Confounding (selection bias) (6 items);
5. Power of the study (1 item).
Studies were graded as excellent quality if their score was between 24-28 points, good if between 19-23 points, fair if between 14-28 points and poor if less than 14 points.
Outcome Measures
The primary outcome measure for this systematic review is the incidence of acute kidney injury (AKI) following cardiac surgery, categorized according to severity stages outlined in the kidney disease: Improving Global Outcomes (KDIGO) guidelines. Secondary outcome measures include evaluating risk factors associated with AKI, assessing preventive strategies' efficacy, analyzing short and long-term clinical outcomes post-AKI, exploring the utility of biomarkers, assessing healthcare resource utilization, documenting adverse events, and performing subgroup analyses to identify potential sources of heterogeneity.
Results
Screening
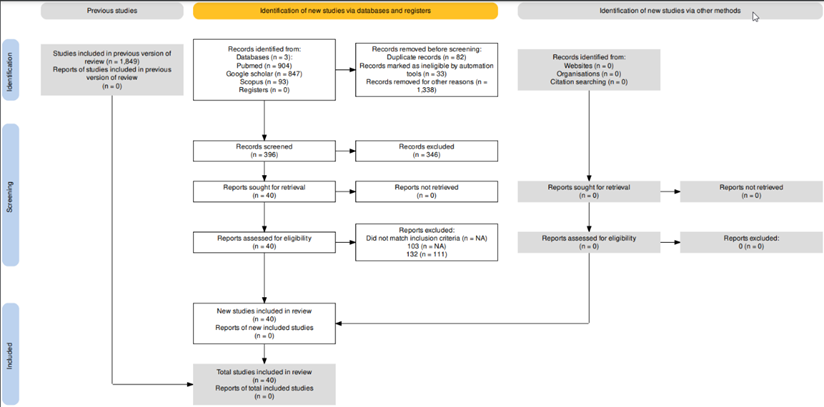
Of 1849 potential studies, 1338 were excluded because they did not assess patients or had titles and abstracts that were not related to the purpose of this review, 82 were excluded because they were duplicates and 33 records were marked as ineligible by automation tools. After careful screening of the remaining 396 articles, 363 were excluded since they fail to meet the inclusion criteria. The 23 retrieved studies were assessed for eligibility. This review is based on the remaining 23 studies that fully met the inclusion criteria.
Table 1: Characteristics of The Studies Included in The Systematic Review.
| S No | Author | Year | Type of study | Sample size | Duration of study | Country | Interventions | Outcomes | Results |
| 1 | David M Axelrod [12] | 2016 | RCT | 144 | USA | Total-2 groups; Aminophylline (n=72); Placebo (n=72) | The primary outcome measure was the development of any AKI, defined by serum creatinine criteria. Secondary outcomes included severe AKI, time to extubating, fluid overload, fluid balance, urine output, bioelectrical impedance, and serum neutrophil gelatinase-associated lipocalin. | This study found no evidence to support the use of postoperative aminophylline in preventing AKI in children recovering from cardiac surgery with cardiopulmonary bypass. | |
| 2 | Pegah Eslami [13] | 2021 | Double blinded RCT | 111 | 7 months | Iran | Total-2 groups; Vit D group (n=50); Control (n=61) | High-dose administration of Vit D may improve the anti-inflammatory state before and after the surgery. However, Vit D pre-treatment was unable to decrease the incidence of AKI and the urinary level of renal biomarkers. | In this study, there was no difference in the occurrence of postop AKI between the Vit D and control groups. However, both urinary levels of IL-18 and kidney injury molecule-1 were elevated after surgery (p lessthan 0.001, for both). Additionally, serum IL-10 levels were increased 3 days after Vit D supplementation (p = 0.001), which was higher than the control group levels post-operation (p lessthan 0.001) and the subsequent day (p = 0.03). |
| 3 | Peter A McCullough [14] | 2016 | RCT | 231 | USA & Denmark | Total-4 groups; Placebo (n=51); ABT 719-800. dose (n= 54); ABT 719- 1600. dose (n=55); ABT 719-2100. dose (n=49) | ABT-719 treatment did not demonstrate efficacy in reducing AKI incidence or influencing biomarker levels in patients undergoing cardiac surgery with cardiopulmonary bypass. | The percentage of patients who developed stage 3 AKI appeared numerically lower in all ABT‐719 groups (5.5percentage for 800, 5.1percentage for 1600, and 5.4percentage for 2100 μg/kg) compared to the placebo arm (12.1percentage), these differences were not statistically significant. | |
| 4 | Madhav Swaminathan [15] | 2018 | RCT | 135 | North America | Total-2 groups; AC 607 (n=68); Placebo (n=67) | The administration of allogeneic mesenchymal stem cells after cardiac surgery within 48 hours of AKI onset did not decrease the time to recovery of kidney function, provision of dialysis or mortality. | The primary analysis of the study found no significant difference in the time to recovery of kidney function between the AC607 and placebo groups. Secondary analysis, including all-cause mortality or provision of dialysis, did not differ significantly between the groups. Twelve patients in the AC607 group and five in the placebo group received dialysis within 30 days of treatment, and 11 patients in the AC607 group and five in the placebo group died within this timeframe. By the end of the study follow-up period, 12 patients in the AC607 group and six in the placebo group had died. | |
| 5 | Mira Küllmar [16] | 2020 | Observational study f/b RCT | 380 | UK | Total -2 groups; Observational group (n=100); Interventional trail (n=100) | The primary endpoint is the compliance rate with the trial protocol. The secondary endpoints including the occurrence of AKI, renal recovery, use of renal replacement therapy, mortality, and safety outcomes. | The single-centre randomized controlled PrevAKI trials demonstrated that the renal biomarkers [TIMP-2] *[IGFBP7] could identify high-risk AKI patients, and the implementation of the CV surgery AKI bundle reduced AKI occurrence by 15percentage. | |
| 6 | Anna J Wetz [17] | 2015 | Observational trail | 342 | Germany | Total -2 groups; NaHCO3 (n= 174); Control (n= 168) | The study observed a significant reduction in the overall incidence of AKI in patients who received sodium bicarbonate treatment. 1. Control group: 50percentage incidence of AKI. 2. NaHCO3 group: 35.6percentage incidence of AKI | Treatment with sodium bicarbonate had a notable impact on reducing the incidence of AKI, particularly in low-risk patients undergoing cardiovascular surgery. The benefits were significant in patients categorized as low risk according to Thakar points (lessthan 3). Sodium bicarbonate can be used as a preventive measure for AKI, with considerations for risk stratification among patients. | |
| 7 | Frederic T Billings IV [18] | 2016 | Double blinded RCT | 615 | 5 years | USA | Total -2 groups and 2 subgroups each. Statin-naïve group: Atorvastatin (n=102); Placebo (n=97). Already on Statin: Atorvastatin (n=206); Placebo (n=210) | Among patients naive to treatment with statins or in patients already taking a statin who are undergoing cardiac surgery, high-dose perioperative atorvastatin treatment compared with placebo did not reduce the risk of AKI. | Among patients naive to statin treatment (n = 199), AKI occurred in 22 of 102 (21.6percentage) in the atorvastatin group vs 13 of 97 (13.4percentage) in the placebo group; Among patients already taking a statin (n = 416), AKI occurred in 42 of 206 (20.4percentage) in the atorvastatin group vs 47 of 210 (22.4percentage) in the placebo group. However, among statin-naïve patients, there was a statistically significant increase in serum creatinine concentration in the atorvastatin group compared to the placebo group. |
| 8 | Jin Sun Cho [19] | 2016 | RCT | 200 | 3 years | South Korea | Total -2 groups; Dexmedetomidine (n=100); Placebo (n=100) | Perioperative infusion of dexmedetomidine effectively lowered both the incidence and severity of AKI and improved overall outcomes in patients undergoing valvular heart surgery, all without any untoward hemodynamic side effects. | The incidence of AKI, as per AKIN criteria, was lower in the treatment group compared to the control group, with rates of 14percentage and 33percentage, respectively. Additionally, the dexmedetomidine group exhibited a significantly reduced incidence of a composite of major morbidity endpoints, with rates of 21percentage compared to 38percentage in the control group. Furthermore, dexmedetomidine group experienced a significantly shorter length of stay in ICU, with a median duration of 2-3 days, compared to 2-4 days in the control group. |
| 9 | Franziska Grundmann [20] | 2018 | RCT | 76 | 3 years | Germany | Total-2 groups; CR group (n=36); Control group (n=40) | The initial results regarding the rise in creatinine levels within the first 24 hours after cardiac surgery were disappointing, the study found positive outcomes at later time, suggest that short-term calorie restriction could have a protective effect in patients at risk for AKI. | The incidence of acute kidney injury (AKI) was reduced by 5.8percentage in the CR group compared to the control group. CR prevented a rise in median creatinine at 48 hours, observed in male patients and with BMI>25. This benefit persisted until discharge, with median creatinine decreasing in the CR group while increasing in the control group. |
| 10 | Thomas Osterholt [21] | 2022 | Double blinded RCT | 115 | Germany | Total-2 groups; Low S group (n=56); Control (n=59) | The outcome of the study suggests that the Low Sulphur diet did not demonstrate a Reno protective effect. | The incidence of AKI within 72 hours after surgery was similar between the Low S group and the control group (23percentage vs. 16percentage; P=0.38). Therefore, while SAA restriction was feasible in the clinical setting, it did not demonstrate protective properties against AKI following cardiac surgery. | |
| 11 | Alexander Zarbock [22] | 2021 | RCT | 278 | Europe | Total-2 groups; Intervention group (n=136); Control group (n=142) | Implementing a treatment bundle based on KDIGO guidelines is achievable across multiple countries. Additionally, the intervention group experienced a notable decrease in moderate to severe AKI. | Within the intervention group, 65.4percentage of patients received the complete bundle, compared to only 4.2percentage in the control group, representing a substantial absolute risk reduction of 61.2percentage. Although overall rates of kidney injury were similar between the groups, the intervention group had notably fewer cases of moderate to severe kidney injury (14.0percentage vs. 23.9percentage). | |
| 12 | Michael Haase [23] | 2013 | RCT | 350 | Germany | Total-2 groups; NaHCO3 (n=174); NaCl control (n=176) | The primary outcome was the proportion of patients developing AKI. Secondary outcomes included assessing the magnitude of acute tubular damage measured by urinary neutrophil gelatinase-associated lipocalin (NGAL), initiation of acute renal replacement therapy, and mortality. | NaHCO3 infusion increased urinary pH but did not reduce the incidence of AKI; instead, more patients receiving NaCHO3 developed AKI compared to the control group and patients receiving NaCHO3 infusion exhibited a greater postoperative increase in urinary NGAL. Additionally, hospital mortality was increased in patients receiving NaCHO3 compared to the control group. | |
| 13 | Adis Tasanarong [24] | 2013 | RCT | 100 | Thailand | Total-2 groups; rHuEPO (n = 50); Placebo (n=50) | The rHuEPO prophylaxis reduced urine NGAL levels within the first three hours following surgery, particularly in patients who developed CSA-AKI, experienced fewer postoperative complications, did not require renal replacement therapy (RRT), and had no deaths. | The incidence of cardiac surgery-associated AKI was lower in the rHuEPO group (14percentage) compared to the placebo group (38percentage; p lessthan 0.01). Postoperative increases in serum creatinine (SCr) and decreases in estimated glomerular filtration rate (eGFR) were significantly lower in the rHuEPO group compared to the placebo group (p lessthan 0.05). | |
| 14 | Francesco Marrazzo [25] | 2019 | RCT | 250 | USA | Total-2 groups; NO gas (n=125); N2-Control (n=125) | The primary outcome is to compare the incidence of AKI between the control and the intervention group. AKI is assessed by evidence of increase in serum creatinine or a decrease in urinary output within 48 hours post-surgery. Secondary outcomes include assessing the severity of AKI is by requirement for renal replacement therapy or worsened renal function at 6 weeks post-surgery. | This study allows for the detection of a 35percentage relative risk reduction in AKI, assuming a two-sided error rate of 0.05 | |
| 15 | Heyman Luckraz [26] | 2021 | RCT | 220 | USA | Total-2 groups; RG group (n=110); Control group (n=110) | In patients who had cardiac surgery with CPB, the RS RG system significantly reduced the incidence of AKI and can be used safely and reproducibly. | The postoperative AKI rates were lower in the RG system group compared to the control group (10percentage vs 20.9percentage; P = 0.025). Additionally, the mean volumes of urine produced during surgery and within the first 24 hours postoperatively were significantly higher in the RG system group (P lessthan 0.001). | |
| 16 | JW Song [27] | 2018 | RCT | 244 | 1 year | South Korea | Total-2 groups; RIC (n=120); Control (n=124) | It seems that repeated RIC do not support to decrease the incidence of AKI after valvular heart surgery. | In this study, perioperative serum creatinine concentrations were similar between the two groups. The incidences of AKI did not significantly differ between the control and RIC groups, with rates of 19.4percentage and 15.8percentagerespectively. |
| 17 | Sun-Kyung Park [28] | 2016 | Observational Study | 220 | 1 year | South Korea | Total -1 group | Patients who developed AKI, younger age (lessthan 12 months), longer CPB time, and low preoperative haemoglobin were independent risk factors. Additionally, an increase in haemoglobin concentration (greaterthan 3 g/dl) from preoperative levels on postoperative day 1 was significantly associated with AKI, regardless of patient demographics and heart disease type. | In a study of paediatric cardiac surgery patients, 41.8percentage developed acute kidney injury (AKI), with 8.2percentage requiring renal replacement therapy within the first postoperative week. AKI severity varied, with 25.9percentage at KDIGO stage 1, 12.3percentage at stage 2, and 3.6percentage at stage 3. Prospective trials are needed to assess whether correcting preoperative anaemia and preventing haemoconcentration can improve outcomes in these patients. |
| 18 | Shahram Amini [29] | 2018 | RCT | 272 | Iran | Total-4 groups; Selenium (n=66); Vitamin C (n=67); NAC (n=68); Control (n=71) | In this study, perioperative administration of N-acetylcysteine, vitamin C and selenium were not effective in preventing acute kidney injury and associated morbidity and mortality after off-pump coronary bypass graft surgery. | In this study involving 272 patients, the overall incidence of acute kidney injury (AKI) was 22.1percentage, with similar rates observed across the vitamin C, NAC, selenium, and control groups (20.9percentage, 22.1percentage, 31.8percentage, and 14.1percentage respectively; P=0.096). The duration of mechanical ventilation, length of stay in the intensive care unit and hospital, and in-hospital mortality did not vary significantly among the four groups. Perioperative administration of NAC, vitamin C or selenium could not reduce the incidence of AKI and its associated mortality and morbidity in patients undergoing off-pump CABG. | |
| 19 | S Soh [30] | 2016 | Double blinded RCT | 162 | Brazil | Total-2 groups; Bicarbonate (n=81); Control (n=81) | Perioperative sodium bicarbonate administration did not decrease the incidence of AKI after off-pump coronary revascularization in high-risk patients and it might be associated with a need for prolonged ventilatory care. | The results indicate no significant difference in the occurrence of AKI between the bicarbonate group (21percentage) and the control group (26percentage) with a p-value of 0.458. However, a notable finding was that more patients in the bicarbonate group required prolonged mechanical ventilation (greaterthan 24 hours) compared to the control group (20 vs. 6), with a significant p-value of 0.003. | |
| 20 | Matthias Thielmann [31] | 2021 | RCT | 341 | North America and Germany | Total-2 groups; Teprasiran (n=176); Placebo (n=165) | The incidence, severity, and duration of early AKI in high-risk patients undergoing cardiac surgery were significantly reduced after Teprasiran administration. | The incidence of acute kidney injury (AKI) was significantly lower in Teprasiran-treated patients compared to those receiving placebo, with rates of 37percentage and 50percentage, respectively, resulting in a 12.8percentage absolute risk reduction (P=0.02) and an odds ratio of 0.58 (95percentage CI, 0.37-0.92). Moreover, AKI severity and duration were improved with Teprasiran, as evidenced by fewer patients experiencing grade 3 AKI (2.5percentage vs. 6.7percentage for Teprasiran vs. placebo) and shorter AKI duration (7percentage vs. 13percentage for Teprasiran vs. placebo patients with AKI lasting ≥5 days). | |
| 21 | Takahiro Moriyama [32] | 2017 | RCT | 48 | Japan | Total -2 groups; hANP (n=24); non hANP (n=24) | In the study, hANP exerted Reno protective effects during cardiac surgery, and can possibly reduce the incidence of AKI after ischemia–reperfusion surgery. Moreover, this protective effect of hANP is mainly induced by inhibition of the intrarenal RAAS. | After cardiac surgery with cardiopulmonary bypass, patients who received hANP had lower levels of urinary angiotensinogen compared to those who did not receive hANP, both immediately after surgery and 3 hours later. At the 3-hour mark post-surgery, hANP-treated patients had lower levels of urinary NGAL, L-FABP. Additionally, it seemed that hANP treatment reduced the incidence of postoperative AKI. | |
| 22 | Melanie Meersch [33] | 2014 | Observational Study | 50 | Germany | Total-1 group | Urinary [TIMP-2] *[IGFBP7] serves as a sensitive and specific biomarker to predict AKI early after cardiac surgery and to predict renal recovery. | In a study of 50 patients undergoing cardiac surgery, 26 patients (52percentage) developed AKI. Urinary concentration of [TIMP-2] *[IGFBP7] increased significantly from a mean of 0.49 (SE 0.24) at baseline to 1.51 (SE 0.57) 4 hours after CPB in AKI patients. The maximum urinary [TIMP-2] [IGFBP7] concentration within the first 24 hours post-surgery demonstrated strong predictive ability for AKI. The decline in urinary [TIMP-2] [IGFBP7] values was identified as the most significant predictor for renal recovery. These findings suggest that urinary [TIMP-2] *[IGFBP7] may serve as an early biomarker for AKI following cardiac surgery and could aid in predicting renal recovery. |
The Overall risk of the included studies was found to be low. Table 2 shows the RoB assessments of individual studies. The mean RoB score was calculated to be 18.29. The mean difference of each study was calculated. Osterholt [10] was found to have the lowest mean difference of -3.7 and the highest RoB score of 22.
Table 2: ROB Using ROBIS Tool.
| S No | Author | Rob Score | Mean Difference |
| 1 | Axelrod DM et al | 18 | 0.2916667 |
| 2 | Eslami P et al | 19 | -0.7083333 |
| 3 | McCullough PA et al | 17 | 1.2916667 |
| 4 | Swaminathan M et al | 18 | 0.2916667 |
| 5 | Kullmar M et al | 21 | -2.7083333 |
| 6 | Wetz AJ et al | 17 | 1.2916667 |
| 7 | Billings FT et al | 17 | 1.2916667 |
| 8 | Cho JS et al | 19 | -0.7083333 |
| 9 | Grundmann F et al | 21 | -2.7083333 |
| 10 | Osterholt T et al | 22 | -3.7083333 |
| 11 | Zarbock et al | 18 | 0.2916667 |
| 12 | Haase M et al | 16 | 2.2916667 |
| 13 | Tasanarong A et al | 18 | 0.2916667 |
| 14 | Marrazzo F et al | 19 | -0.7083333 |
| 15 | Luckraz H et al | 20 | -1.7083333 |
| 16 | Song JW et al | 21 | -2.7083333 |
| 17 | Park SK et al | 19 | -0.7083333 |
| 18 | Amini S et al | 18 | 0.2916667 |
| 19 | Soh S et al | 17 | 1.2916667 |
| 20 | Thielmann M et al | 18 | 0.2916667 |
| 21 | Moriyama T et al | 17 | 1.2916667 |
| 22 | Gocze I et al | 16 | 2.2916667 |
| 23 | Meersch M et al | 17 | 1.2916667 |
| Mean score | 18.2916667 |
Tabulation of mean difference and confidence intervals.
| Alpha | |
| Standard Deviation | 1.706233244 |
| Population Size | 23 |
| Confidence Interval | 0.682622925 |
| Study | Mean Difference | CI+ | CI- |
| Axelrod DM | 0.2916667 | 0.6206667 | -0.0373333 |
| Eslami P | -0.7083333 | -0.3793333 | -1.0373333 |
| McCullough PA | 1.2916667 | 1.6206667 | 0.9626667 |
| Swaminathan M | 0.2916667 | 0.6206667 | -0.0373333 |
| Kullmar M | -2.7083333 | -2.3793333 | -3.0373333 |
| Wetz AJ | 1.2916667 | 1.6206667 | 0.9626667 |
| Billings FT | 1.2916667 | 1.6206667 | 0.9626667 |
| Cho JS | -0.7083333 | -0.3793333 | -1.0373333 |
| Grundmann F | -2.7083333 | -2.3793333 | -3.0373333 |
| Osterholt T | -3.7083333 | -3.3793333 | -4.0373333 |
| Zarbock | 0.2916667 | 0.6206667 | -0.0373333 |
| Haase M | 2.2916667 | 2.6206667 | 1.9626667 |
| Tasanarong A | 0.2916667 | 0.6206667 | -0.0373333 |
| Marrazzo F | -0.7083333 | -0.3793333 | -1.0373333 |
| Luckraz H | -1.7083333 | -1.3793333 | -2.0373333 |
| Song JW | -2.7083333 | -2.3793333 | -3.0373333 |
| Park SK | -0.7083333 | -0.3793333 | -1.0373333 |
| Amini S | 0.2916667 | 0.6206667 | -0.0373333 |
| Soh S | 1.2916667 | 1.6206667 | 0.9626667 |
| Thielmann M | 0.2916667 | 0.6206667 | -0.0373333 |
| Moriyama T | 1.2916667 | 1.6206667 | 0.9626667 |
| Gocze I | 2.2916667 | 2.6206667 | 1.9626667 |
| Meersch M | 1.2916667 | 1.6206667 | 0.9626667 |
Discussion
Acute kidney injury (AKI) remains a significant and frequently encountered complication following cardiac surgery, presenting a formidable challenge to patient recovery and prognosis. This systematic review underscores the substantial burden of cardiac surgery-associated AKI (CSA-AKI), with reported incidence rates ranging from 14% to 50percentage across the included studies [8,13,19]. This variability likely arises from the heterogeneity in patient characteristics, surgical procedures, and diagnostic criteria employed. Nonetheless, these findings align with previous meta-analyses and large-scale observational studies, collectively highlighting the pervasive nature of this complication and the urgent need for effective preventive and therapeutic interventions [1,2]. Finding targeted treatments for CSA-AKI is extremely difficult due to its complex etiology, which includes ischemia-reperfusion injury, inflammation, oxidative stress, and hemodynamic disturbances. With varying degrees of success, a number of pharmacological treatments targeted at reducing these underlying mechanisms were assessed. Vitamin C, aminophylline [1], N-acetylcysteine, selenium [18], and vitamin C were among the agents that did not show a discernible decrease in the incidence or severity of AKI. These results are in line with earlier systematic reviews and meta-analyses [3,4], indicating that these medications might not be able to sufficiently address the intricate pathophysiological mechanisms driving CSA-AKI. On the other hand, encouraging outcomes were noted when dexmedetomidine, a highly selective α2-adrenergic receptor agonist, was administered during surgery [8]. According to Cho et al.'s study, the dexmedetomidine group had reduced incidence and severity of AKI, which may have been caused by the drug's pleiotropic effects, which include anti-inflammatory, anti-apoptotic, and Reno protective qualities [5]. Reno protective properties of dexmedetomidine are demonstrated by its ability to reduce ischemia-reperfusion injury and inflammatory cascades related to heart surgery.
Two promising non-pharmacological strategies to reduce CSA-AKI are the use of a revolutionary renal guard (RG) system [15] and the introduction of a KDIGO-based treatment bundle [11]. Moderate to severe AKI patients were significantly reduced as a result of the treatment bundle, which included strategies like avoiding nephrotoxic substances, optimizing fluid management, and initiating renal replacement therapy as soon as possible. This result emphasizes how crucial it is to implement multidisciplinary care protocols and evidence-based standards in order to improve renal outcomes. Comparably, the RG system showed a decreased incidence of AKI and enhanced urine production. The RG system was created to lessen the hemodynamic and inflammatory insults associated with cardiopulmonary bypass (CPB). Larger, multicenter trials should be conducted to confirm the clinical value and cost-effectiveness of this innovative technology, as these encouraging results demand for. Teprasiran, a new P2Y12 receptor antagonist, was found to significantly reduce the frequency and severity of AKI [20]. This is a noteworthy finding from the review. When adenosine diphosphate (ADP) activates the P2Y12 receptor, which is present on platelets and different types of vascular cells, it plays a crucial part in thrombosis and inflammation [7]. Teprasiran may have Reno protective effects by blocking this receptor, which would lessen the inflammatory cascade and microvascular dysfunction linked to CPB. These results underline the possibility of targeted therapeutics regulating this system and are consistent with the increasing understanding of the role of purinergic signaling in AKI development.
Because novel biomarkers like urine NGAL, plasma NGAL (pNGAL), and the urinary [TIMP-2] × [IGFBP7] product are predictively beneficial in identifying people at risk, there is hope for early intervention and prevention of CSA-AKI [8,9,22,23]. These indicators have demonstrated improved diagnostic efficacy when compared to traditional markers such serum creatinine, enabling the early detection of renal disease. By identifying high-risk individuals early on, appropriate preventive interventions and tighter monitoring can be put in place, potentially delaying the onset and severity of AKI. Meersch et al.'s work [23] further highlighted the potential clinical utility of urine [TIMP-2] × [IGFBP7], as it showed the ability to predict both the development of AKI and renal recovery. The results of this review further highlight the significance of customized preventative measures and risk stratification. Wetz et al.'s study [6] showed that sodium bicarbonate therapy is effective in lowering the incidence of AKI, especially in low-risk patients after heart surgery. On the other hand, patients who are more likely to develop AKI may benefit more from short-term calorie restriction, according to research by Grundmann et al. [9]. These results are consistent with the increasing awareness that, considering the variety of risk profiles and underlying comorbidities of patients undergoing heart surgery, a "one-size-fits-all" strategy may not be the most effective in reducing CSA-AKI. Customizing preventative measures according to personal risk evaluations could improve their efficiency and best use of available resources. There is ample evidence of the negative effects of CSA-AKI, such as higher mortality, longer hospital admissions, and higher healthcare expenditures; yet, one major obstacle continues to be the lack of consistently effective therapies. This gap emphasizes the necessity of investigating new therapeutic targets and strategies in addition to gaining a better knowledge of the intricate pathophysiological mechanisms underlying the development of AKI in the setting of cardiac surgery.
Future studies could examine targeted therapeutics that modulate particular pathways implicated in the pathophysiology of CSA-AKI, such as the purinergic signaling system that Teprasiran targets. Furthermore, more research is necessary to fully understand the significance of cutting-edge therapeutic approaches including gene therapy and cell-based therapies in the prevention and treatment of CSA-AKI. Although the administration of allogeneic mesenchymal stem cells was not shown to be effective in the trial by Swaminathan et al. [4], it does show that cell-based therapies have the capacity to modulate the inflammatory and regenerative processes involved in AKI. Moreover, the incorporation of innovative biomarkers and risk assessment instruments into clinical decision-making algorithms could expedite the execution of customized preventive and therapeutic approaches. Early identification of high-risk patients and customized interventions based on individual risk profiles may enhance treatment outcomes and the efficacy of preventive measures. The research conducted by Gocze et al. [22] and Meersch et al. [23] offers valuable perspectives on the possible use of the urinary [TIMP-2] × [IGFBP7] biomarker in risk assessment and renal recuperation tracking, respectively. Finally, this systematic review offers a thorough summary of the state of CSA-AKI today, emphasizing the problems that still need to be solved and possible directions for further investigation. The lack of consistently effective medicines highlights the need for ongoing research efforts, even if a number of interventions and methods, like the injection of dexmedetomidine, KDIGO-based treatment bundles, novel biomarkers, and targeted medications like Teprasiran, have showed promise. To reduce the significant burden connected with this consequence and enhance patient outcomes, it is imperative to clarify the intricate pathophysiological mechanisms underlying CSA-AKI and create tailored, focused preventative and therapy strategies.
Limitations
Variability in study designs, patient populations, and interventions across included studies may contribute to heterogeneity. Despite quality assessment, the variability in methodological quality among included studies introduce bias and affect the robustness of the findings. The findings of the systematic review may not be fully generalizable to all patient populations or healthcare settings. The availability of high-quality interventional studies targeting AKI prevention or management post-cardiac surgery were limited, potentially restricting the ability to make firm recommendations for clinical practice.
Conclusion
In conclusion, this systematic review sheds light on the significant burden of acute kidney injury (AKI) following cardiac surgery, emphasizing its detrimental impact on patient outcomes and healthcare systems. Despite advancements in surgical techniques and perioperative care, the incidence of AKI remains substantial, necessitating targeted interventions to mitigate its occurrence. While pharmacological agents such as aminophylline, vitamin C, and selenium did not demonstrate significant efficacy in reducing AKI, promising results were observed with dexmedetomidine administration, the use of renal guard systems, and implementation of KDIGO-based treatment bundles. Furthermore, novel therapeutics like Teprasiran show potential in reducing the frequency and severity of AKI, providing hope for targeted interventions to alleviate the inflammatory cascades and microvascular dysfunction associated with cardiac surgery. Additionally, the identification of early biomarkers such as urinary NGAL and [TIMP-2] × [IGFBP7] offers opportunities for early intervention and preventive strategies, enabling clinicians to identify high-risk individuals and initiate timely interventions. Overall, this review underscores the complexity of AKI pathophysiology, the need for multidisciplinary approaches, and the importance of evidence-based standards in improving renal outcomes post-cardiac surgery. Future research should focus on conducting larger, multicenter trials to validate the efficacy and cost-effectiveness of innovative technologies and therapeutic interventions, ultimately enhancing patient care and reducing the burden of AKI on healthcare systems.
References
- Susantitaphong P., Cruz D.N., Cerda J., et. al. (2013). World Incidence of AKI: A Meta-Analysis. Clin J Am Soc Nephrol. 8:1482-1493.
Publisher | Google Scholor - Pickering JW, James MT, Palmer SC. (2015). Acute Kidney Injury and Prognosis After Cardiopulmonary Bypass: A Meta-Analysis of Cohort Studies. Am J Kidney Dis. 65(2):283-293.
Publisher | Google Scholor - Bellomo R., Ronco C., Kellum J.A., Mehta R.L., Palevsky P.M. (2004). Acute Dialysis Quality Initiative Workgroup Acute Renal Failure—Definition, Outcome Measures, Animal Models, Fluid Therapy and Information Technology Needs: The Second International Consensus Conference of The Acute Dialysis Quality Initiative (ADQI) Group. Crit Care. 8:204-212.
Publisher | Google Scholor - Mehta R.L., Kellum J.A., Shah S.V. et al. (2007). Acute Kidney Injury Network: Report of An Initiative to Improve Outcomes in Acute Kidney Injury. Crit Care. 11:31.
Publisher | Google Scholor - KDIGO. (2012). Clinical Practice Guideline for Acute Kidney Injury Section 2: AKI Definition. Kidney Int Suppl. 1:19-36.
Publisher | Google Scholor - Boldt J, Brenner T, Lehmann A, Suttner SW, Kumle B, et al. (2003). Is Kidney Function Altered by The Duration of Cardiopulmonary Bypass? Ann. Thorac. Surg. 75(3):906-912.
Publisher | Google Scholor - Rosner, M.H., Okusa, M.D. (2006). Acute Kidney Injury Associated with Cardiac Surgery. Clin. J. Am. Soc. Nephrol. 1:19-32.
Publisher | Google Scholor - Haase M, Bellomo R, Devarajan P, Schlattmann P, Haase-Fielitz A. (2009). Accuracy Of Neutrophil Gelatinase-Associated Lipocalin (NGAL) In Diagnosis and Prognosis in Acute Kidney Injury: A Systematic Review and Meta-Analysis. Am. J. Kidney Dis. 54(6):1012-1024.
Publisher | Google Scholor - Greenwood, S. A., Mangahis, E., Castle, E. M., Wang, J., Campbell, J., et al. (2019). Arterial Stiffness Is a Predictor for Acute Kidney Injury Following Coronary Artery Bypass Graft Surgery. Journal of Cardiothoracic Surgery, 14.
Publisher | Google Scholor - Legouis D, Galichon P, Bataille A, Chevret S, Provenchère S, et al. (2017). Rapid Occurrence of Chronic Kidney Disease in Patients Experiencing Reversible Acute Kidney Injury After Cardiac Surgery. Anesthesiology. 126(1):39-46.
Publisher | Google Scholor - National Confidential Enquiry into Patient Outcomes and Death (NCEPOD) Report: Adding Insult to Injury. (2009).
Publisher | Google Scholor - Axelrod, David M., et al. (2016). A Double-Blinded, Randomized, Placebo-Controlled Clinical Trial of Aminophylline to Prevent Acute Kidney Injury in Children Following Congenital Heart Surgery with Cardiopulmonary Bypass. Pediatric Critical Care Medicine. 17(2):135-143.
Publisher | Google Scholor - Eslami, Pegah, et al. (2021). A Randomized, Double-Blind, Placebo-Controlled, Clinical Trial of High-Dose, Short-Term Vitamin D Administration in The Prevention of Acute Kidney Injury After Cardiac Surgery. Cardiorenal Medicine. 11(1):52-58.
Publisher | Google Scholor - McCullough, Peter A., et al. (2016). ABT‐719 for the prevention of acute kidney injury in patients undergoing high‐risk cardiac surgery: a randomized phase 2b clinical trial. Journal of the American Heart Association. 5(8):e003549.
Publisher | Google Scholor - Swaminathan, Madhav, et al. (2018). Allogeneic mesenchymal stem cells for treatment of AKI after cardiac surgery. Journal of the American Society of Nephrology. 29(1):260-267.
Publisher | Google Scholor - Küllmar, Mira, et al. (2020). Biomarker-Guided Implementation of The KDIGO Guidelines to Reduce the Occurrence of Acute Kidney Injury in Patients After Cardiac Surgery (Prev AKI-Multicenter): Protocol for A Multicenter, Observational Study Followed by Randomized Controlled Feasibility Trial. BMJ Open. 10(4):e034201.
Publisher | Google Scholor - Wetz, Anna J., et al. (2015). Does Sodium Bicarbonate Infusion Really Have No Effect on The Incidence of Acute Kidney Injury After Cardiac Surgery? A Prospective Observational Trial. Critical Care. 19:1-10.
Publisher | Google Scholor - Billings, Frederic T., et al. (2016). High-Dose Perioperative Atorvastatin and Acute Kidney Injury Following Cardiac Surgery: A Randomized Clinical Trial. Jama. 315(9):877-888.
Publisher | Google Scholor - Cho, Jin Sun, et al. (2016). Perioperative Dexmedetomidine Reduces the Incidence and Severity of Acute Kidney Injury Following Valvular Heart Surgery. Kidney International. 89(3):693-700.
Publisher | Google Scholor - Grundmann, Franziska, et al. (2018). Preoperative Short‐Term Calorie Restriction for Prevention of Acute Kidney Injury After Cardiac Surgery: A Randomized, Controlled, Open‐Label, Pilot Trial. Journal of the American Heart Association. 7(6):e008181.
Publisher | Google Scholor - Osterholt, Thomas, et al. (2022). Preoperative Short‐Term Restriction of Sulfur‐Containing Amino Acid Intake for Prevention of Acute Kidney Injury After Cardiac Surgery: A Randomized, Controlled, Double‐Blind, Translational Trial. Journal of the American Heart Association. 11(17):e025229.
Publisher | Google Scholor - Zarbock, Alexander, et al. (2021). Prevention Of Cardiac Surgery–Associated Acute Kidney Injury by Implementing the KDIGO Guidelines in High-Risk Patients Identified by Biomarkers: The PrevAKI-Multicenter Randomized Controlled Trial. Anesthesia and Analgesia. 133(2):292-302.
Publisher | Google Scholor - Haase, Michael, et al. (2013). Prophylactic Perioperative Sodium Bicarbonate to Prevent Acute Kidney Injury Following Open Heart Surgery: A Multicenter Double-Blinded Randomized Controlled Trial. PLoS. 10(4):e1001426.
Publisher | Google Scholor - Tasanarong, Adis, et al. (2013). Prophylaxis With Erythropoietin Versus Placebo Reduces Acute Kidney Injury and Neutrophil Gelatinase-Associated Lipocalin in Patients Undergoing Cardiac Surgery: A Randomized, Double-Blind Controlled Trial. BMC Nephrology. 14:1-10.
Publisher | Google Scholor - Marrazzo, Francesco, et al. (2019). Protocol of a Randomized Controlled Trial in Cardiac Surgical Patients with Endothelial Dysfunction Aimed to Prevent Postoperative Acute Kidney Injury by Administering Nitric Oxide Gas. BMJ Open. 9(7):e026848.
Publisher | Google Scholor - Luckraz, Heyman, et al. (2021). Reduction In Acute Kidney Injury Post Cardiac Surgery Using Balanced Forced Diuresis: A Randomized, Controlled Trial. European Journal of Cardio-Thoracic Surgery. 59(3):562-569.
Publisher | Google Scholor - Song, J. W., et al. (2018). Remote Ischemic Conditioning for Prevention of Acute Kidney Injury After Valvular Heart Surgery: A Randomized Controlled Trial. British Journal of Anesthesia. 121(5):1034-1040.
Publisher | Google Scholor - Park, Sun-Kyung, et al. (2016). Risk Factors for Acute Kidney Injury After Congenital Cardiac Surgery in Infants and Children: A Retrospective Observational Study. PLoS One. 11(11):e0166328.
Publisher | Google Scholor - Amini, Shahram, et al. (2018). Selenium, Vitamin C And N-Acetylcysteine Do Not Reduce the Risk of Acute Kidney Injury After Off-Pump CABG: A Randomized Clinical Trial. Brazilian Journal of Cardiovascular Surgery. 33:129-134.
Publisher | Google Scholor - Soh, S., et al. (2016). Sodium Bicarbonate Does Not Prevent Postoperative Acute Kidney Injury After Off-Pump Coronary Revascularization: A Double-Blinded Randomized Controlled Trial. BJA: British Journal of Anaesthesia. 117(4):450-457.
Publisher | Google Scholor - Thielmann, Matthias, et al. (2021). Teprasiran, A Small Interfering RNA, For the Prevention of Acute Kidney Injury in High-Risk Patients Undergoing Cardiac Surgery: A Randomized Clinical Study. Circulation. 144(14):1133-1144.
Publisher | Google Scholor - Moriyama, Takahiro, et al. (2017). The Protective Effect of Human Atrial Natriuretic Peptide on Renal Damage During Cardiac Surgery. Journal of anesthesia. 31:163-169.
Publisher | Google Scholor - Meersch, Melanie, et al. (2014). Urinary TIMP-2 and IGFBP7 as early biomarkers of acute kidney injury and renal recovery following cardiac surgery. PloS One. 9(3):e93460.
Publisher | Google Scholor